John J. Martin describes the options available to practitioners when addressing the medial lower eyelid as well as his personal approach with fillers

a board certified ophthalmologist, is a cosmetic plastic surgeon specializing in eyelid, brow, facial, and neck rejuvenation.
email: [email protected]
One of the more commonly requested oculoplastic procedures today is the injection of fillers into the lower eyelid tear trough. Hollowing in this area is typically associated with dark circles that cause individuals to appear fatigued. There are many factors that contribute to the dark circles, most importantly, genetics and the underlying anatomy. When evaluating the lower eyelid, the main area of initial focus should be the tear trough.
The tear trough or nasojugal groove is the natural depression extending inferolaterally from the medial canthus. The palpebromalar groove runs along the lateral half of the orbital rim and is continuous with the tear trough. The groove is formed by the orbital retaining ligament laterally and the tear trough ligament medially. As described by Wong et al. in 2012, these osteocutaneous ligaments are located between the palpebral and orbital parts of the orbicularis oculi muscle1. With ageing, the groove may become more apparent and deepen further. In addition, the orbital fat may move forward, creating increased shadowing of the tear trough, making it appear even darker. There may also be a descent of the midface and malar fat pads, creating exposure of the inferior orbital rim. Additional factors that can worsen lower lid appearance include loss of bone, and skin changes and loss of dermal collagen from solar damage. Lambros also described lower eyelid skin atrophy, which leads to a darkening of the preseptal skin2. This will increase the contrast and accentuate the lid/cheek junction.
Many young people will also develop dark circles that are unrelated to ageing. In these patients, congenital malar hypoplasia results in a tear trough volume deficit, so the lower lid will appear hollow and dark. Some will also have increased pigmentation in the lower lid, which will worsen the appearance of the dark circle.
One of the best non-surgical ways to improve the appearance of a lower lid with tear trough hollowing is with the addition of filler. Hyaluronic acid gels (HAG) have been used since 2006 for rejuvenation of the periorbital hollows3–6. The addition of HAG provides increased volume to the tear trough, which decreases the shadowing and smooths out the transition from the cheek into the lower lid. The addition of volume will also elevate and stretch the skin, helping to decrease the appearance of the darker pigmentation if that is present. An advantage to HAG over other types of fillers is that it can be dissolved with the injection of hyaluronidase if the patient is unhappy with the result. Most clinical studies have reported high patient satisfaction with the use of periorbital HAG fillers, 89% by Goldberg3, 92% by Beruiga7, and 97% by Lipp8.
Available fillers
There are many commercially available FDA approved hyaluronic acid gels; however, the use of fillers in the periocular area is considered ‘off label’. Most clinicians use one of the thinner, less hydrophilic gels in the tear trough, as these are associated with lower rates of periorbital oedema, dyschromia, and visible irregularities when compared to more hydrophilic gels.
Two of the more popular, less hydrophilic HAG choices for the tear trough are Restylane-L and Belotero Balance. Clinical studies using Restylane have shown high patient satisfaction with a low incidence of complications3–5,9. Belotero is another popular HA filler for the tear trough given its low elasticity and viscosity and soft flowing qualities. It is not very hydrophilic, so it will usually not result in significant post-injection oedema10. Belotero does not contain lidocaine, but this may be added to the filler prior to injection.
Most injectors will avoid using HAGs that are highly hydrophilic, such as Juvederm, as these can create long term oedema in this area11. While Voluma, one of the thicker fillers, is not usually chosen for tear trough injections, Hall et al. studied Voluma injections in the tear trough of 202 eyes without reports of significant oedema12.
Radiesse is also not used often in the tear trough. It is a non-HAG filler, made of calcium hydroxyapatite gel microspheres.
Bernardini et al. injected Radiesse into the tear trough of 63 patients and reported high patient satisfaction, minimal complications, and no nodule formation13. The main risk of using a non-HAG product such as CaHA is that they cannot be dissolved if the patient is unhappy with the result. Nodules that develop need to be surgically removed.
Techniques and procedure
Most injectors recommend filling below the orbicularis and just above the periosteum3,4. Placement of the filler in this deep plane should decrease the possibility of visible irregularities, and also decrease the risk of intravascular injection. When placed at the periosteum, the results are usually evident for at least 12 months. Most injectors will begin with 1 cc of HA filler, which is used to fill both tear troughs. If a patient has a very deep trough more may be needed, which can be done at the time or at a subsequent visit.
There are a variety of injection techniques, including linear threading with either anterograde or retrograde injections, serial puncture, and depot injections8. With linear threading antegrade injections, there will be hydrodissection of the tissue that creates a plane to deposit the filler. It will also provide anaesthesia to the tissue as the needle or cannula is advanced. With retrograde injections, the filler will be placed into the tracks as the needle or cannula is withdrawn. With both techniques, the needle or cannula is continually moving, which will help to decrease the risk of intravascular occlusion.
With serial puncture, small volumes are injected along the length of the tear trough.
The repeated needle entry points may increase the risk of bruising. It allows for more superficial injections if desired. Depot injections are performed just above the bone, and these can be spaced out along the tear trough, or one large injection may be done and then massaged out14. Some clinicians will also use a more superficial placement of filler. However, the superficial location could make the filler or any irregularities more visible, and it may compromise lymphatic drainage more than deep injections, causing malar oedema15.
Both needles and cannulas can be used to fill the tear trough, and this is dependent on the injectors’ preference. Cannulas may help to decrease bruising as only one entry point is made for the cannula, and this is usually inferolateral to the eyelid. They may also decrease the risk of intravascular injection16.

This author’s preference is to use a 25-gauge cannula with an entry point inferolateral to the eyelid. I will inject Belotero with 0.2 cc of lidocaine added to a 1 cc tube, or Restylane-L. For patients with very thin skin, I will dilute a 1 cc tube of Restylane with 0.4 cc of normal saline. I will initially fill just above the periosteum. I will then also go in a more superficial plane to deposit additional filler. By diluting the product, it is very easily smoothed out with an applicator, and the blue-grey discolouration reported with superficial injections is rarely seen.
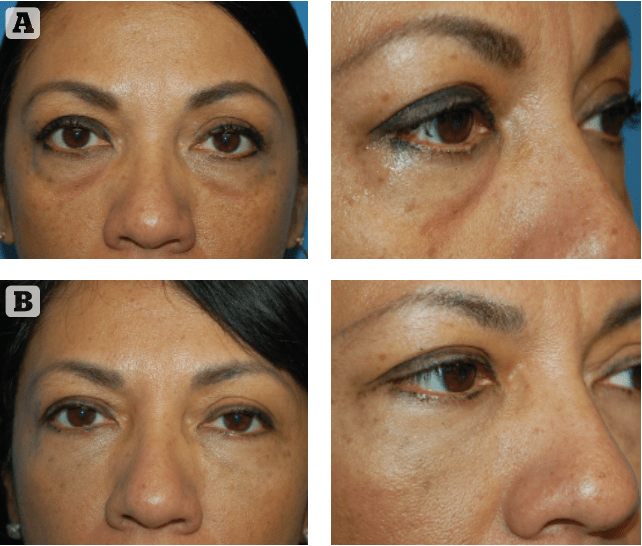
The superficial placement also provides additional stretch to the skin, which can help decrease the appearance of dark circles in patients with increased pigmentation in this area. A clinical example of a patient with HA filler injected with a cannula is seen in Figure 1.
Prior to tear trough injections, patients should stop any anti-coagulant medications or vitamins if possible. The skin should be prepped thoroughly with anti-bacterial preparations. Topical anaesthesia can be applied beforehand, and vibration anaesthesia is an excellent way to decrease any discomfort during the procedure. If a bruise occurs, pressure should be placed over the area immediately. This will help to prevent the spread of the bruise and hopefully allow sufficient visibility of the anatomy to complete the injections.
Upper cheek
If a patient has also lost volume in the upper cheek, it is usually recommended that this area receives filler first as it may change the contour of the lower lid and tear trough. However, as reported by Hill et al., if the patient’s primary concern is the tear trough, and they elect to treat only one area (just the tear trough or the cheek) a better cosmetic result is obtained by injecting the tear trough as opposed to the cheek17.
It is important for the patient to have realistic expectations when adding volume to the tear trough. Patients with very large fat pads may not get much improvement, and surgery will be a better option. Large amounts of wrinkled skin may also not improve dramatically. And very dark skin may only see modest improvement. For patients with darker skin in the tear trough, there are many options that may help in addition to fillers. These include concealers, topical bleaching agents, retinoids, peels, and lasers18.
Complications
The more common complications seen with HAG fillers are lower eyelid or malar oedema, blue-grey dyschromia, contour irregularities, and bruising19. Most of these are mild and no treatment is needed.
If the patient is unhappy with the result, or if there is an overcorrection, hyaluronidase can be injected to dissolve the filler. There have been rare instances of foreign body granuloma formation with HAG filler20. Skin necrosis and blindness from intravascular occlusion are also very rare in this area21.
Conclusions
The use of hyaluronic acid gel fillers to add volume to a lower eyelid is an excellent option for patients with dark circles who have a deep tear trough. Adding filler to the tear trough is an advanced injection technique and should only be done by experienced injectors. For patients with dark circles, there are many advantages to using HAG fillers in this area: a non-surgical procedure, high degree of patient satisfaction, minimal complications, and its reversibility with hyaluronidase.
Declaration of interest I would like to thank Kathryn A Martin, MD for her writing assistance and editing of the manuscript.
Figures 1 © Dr Martin
References
- Wong CH, Hsieh MK, Mendelson B. The tear trough ligament; anatomical basis for the tear trough deformity. Plast Reconstr Surg. 2012;129(6):1392-402
- Lambros V. Observations on periorbital and midface aging. Plast Reconstr Surg. 2007;120(5):1367-76
- Goldberg RA, Fiaschetti D. Filling the periorbital hollows with hyaluronic acid gel: initial experience with 244 injections. Ophthal Plast Reconstr Surg. 2006;22(5): 335-41
- Steinsapir KD, Steinsapir SM. Deep-fill hayluronic acid for the temporary treatment of the nasojugal groove: a report of 303 consecutive treatments. Ophthal Plast Reconstr Surg. 2006;22(5): 344-8
- Sharad, J. Dermal Fillers for the Treatment of Tear Trough Deformity: A Review of Anatomy, Treatment Techniques, and their Outcomes. J Cutan Aesthet Surg. 2012;5(4):229-38
- Lee S, Yen MT. Nonsurgical Rejuvenation of the Eyelids with Hyaluronic Acid Gel Injections. Semin Plast Surg. 2017;31(1):17-21
- Berguiga M, Galatoire O. Tear Trough rejuvenation: A safety evaluation of the treatment by a semi-cross-linked hyaluronic acid filler. Orbit. 2017; 36(1):22-26
- Lipp M, Weiss E. Nonsurgical Treatments for Infraorbital Rejuvenation: A Review. Dermatol Surg. 2019;45(5):700-710
- Viana GAP, Osaki MH, Cariello AJ, Damasceno RW, Osaki TH. Treatment of the Tear Trough Deformity with Hyaluronic Acid. Aesthet Surg J. 2011;31(2):225-231
- Huber-Vorlander J, Kurten M. Correction of tear trough deformity with a cohesive polydensified matrix hyaluronic acid: a case series. Clin Cosmet Investig Dermatol. 2015;8:307-312
- Iverson SM, Patel RM. Dermal filler-associated malar edema: Treatment of a persistent adverse effect. Orbit. 2017; 36(6): 473-475
- Hall MB, Roy S. Buckingham ED. Novel Use of a Volumizing Hyaluronic Acid Filler for Treatment of Infraorbital Hollows. JAMA Facial Plast Surg. 2018;20(5):367-372
- Bernardini FP, Devoto MH, Cetinkaya A, Zambelli A. Calcium hydroxyl-apatite (Radiesse) for the correction of periorbital hollows, dark circles, and lower eyelid bags. Ophthal Plast Reconstr Surg. 2014;30(6): 34-39
- Friedmann DP, Goldman MP. Dark Circles. Clin Plast Surg. 2015 Jan;42(1): 33-50
- Pascali M, Quarato D, Pagnoni M, Carinci F. Tear Trough Deformite: Study of Filling Procedures for Its Corrections. J Craniofac Surg 2019;28:2012-2015
- Bertucci V, Lynde CB. Current Concepts in the Use of Small-Particle Hyaluronic Acid. Plast Reconstr Surg. 2015;136(5S):132S-138S
- Hill RH, Czyz CN, Kandapalli S, Zhang-Nunes SX, Cahill KV, Wulc AE, Foster JA. Evolving Minimally Invasive Techniques for Tear Trough Enhancement. Ophthal Plast Reconsrt Surg. 2015; 31(4):306-309
- Vrcek I, Ozgur O, Nakra t. Infraorbital Dark Circles: a Review of the Pathogenesis, Evaluation and Treatment. J Cutan Aesthet Surg. 2016;9(2):65-72
- Mustak H, Fiaschetti D, Goldberg RA. Filling the periorbital hollows with hyaluronic acid gel: Long-term review of outcomes and complications. J Cosmet Dermatol. 2018;17:611-616
- Parulan MAA, Sundar G, Lum JH, Ramachandran U. A case report on dermal filler-related periorbital granuloma formation. Orbit. 2019;38(2):169-172
- Beleznay K, Carruthers JD, Humphrey S, Jones D. Avoiding and Treating Blindness From Fillers: A Review of the World Literature. Dermatol Surg 2015;41(10):1097-117