Jamuna Pai discusses lip enhancement using hyaluronic acid fillers, including study results and individual cases
Fuller lips have been synonymous with beauty and youth since the beginning of recorded history. Humans have adorned their lips as far back as the ancient Egyptians. Some societies still go to great lengths to draw attention to their lips1. Variation in lip anatomy follows racial predisposition, which is evident when observing different races. The ideal vertical height ratio or the ‘golden ratio’ of the upper to lower lip as defined by the ancient Greeks is 1:1618 in youthful Caucasian lips2. Individuals of African descent have genetically more volume on their lips. However, while creating ‘perfect lips’, there is no fixed definition or criteria, and it is up to the skills of the medical practitioner and the expectations of the individual. Therefore, in order to create aesthetically beautiful lips a thorough understanding of the underlying anatomy of the region is vital in planning a treatment strategy.
Lip anatomy
The skin of the perioral region is stratified squamous epithelium and consists of the epidermis, dermis, and hypodermis. It contains hair follicles as well as sebaceous and sweat glands and is separated from the underlying tissue by connective tissue and muscles. On the inner side of the lip lies the mucosa with multiple salivary glands called labial glands3,4.
Muscles of the perioral region
T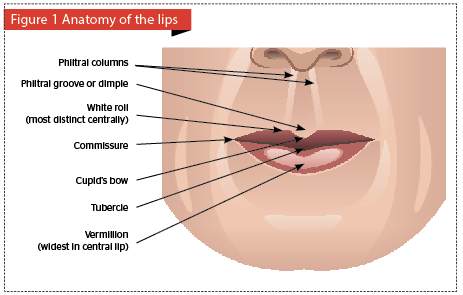
The aesthetic upper lip has a ‘Flattened M’ configuration at the vermilion-cutaneous junction or border, commonly referred to as ‘Cupid’s Bow’. The mucosa, or vermilion, consists of both a ‘dry’ and ‘wet’ portion. This junction has a ‘white roll’, which is a defining outline and the result of light reflection from this area5.The vermilion is red due to the absence of keratin and the closely underlying rich vascular plexus.
Blood and nerve supply
The muscles of the lips receive motor innervation from the facial nerve and sensory innervation from the maxillary (V2) and mandibular (V3) branches of the trigeminal nerve. The blood supply to both lips is via the inferior and superior labial arteries. These branches of the facial artery are located deep to the mucosa and the orbicularis oris muscle6. The facial artery branches into the superior labial artery just above the labial commissure. It runs 4.5 mm deep along the upper lip between the oral mucosa and the orbicularis oris muscle just above the vermillion-mucosa junction to anastomosis with the opposing artery. The inferior labial artery, meanwhile, originates as a common trunk along with the labiomental artery where the facial artery enters the oral vestibule deep to the platysma muscle. The main arterial trunk courses along the alveolar border within the plane between the orbicularis oris muscle and the lip depressors. From the arterial trunk emanates the inferior labial artery, which accompanies the mental nerve to the lower lip.
Vasculature
Although the vascular anatomy of the lips does vary from person to person and most of the arteries are not symmetrical, a better understanding of the common patterns of the labial arteries is helpful when performing any treatment in this area (Figure 2).
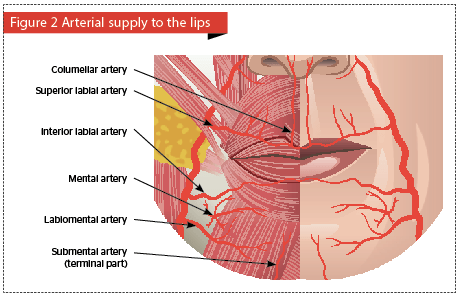
The blood supply of the lower lip is supplied via the facial artery and its three branches. The first artery courses along the margin of the inferior lip and, therefore, is known as the ‘inferior labial artery’; the second traverses the labiomental portion horizontally — the ‘horizontal labial artery’; and the third runs vertically through the labiomental portion — the ‘vertical labial artery’7.
Ageing lips
In order to have the right treatment plan, it is first important to understand the role that ageing plays on lips and the perioral region. Youthful perioral skin is smooth with minimal nasolabial folds and little to no rhytids. With time, the lips atrophy and thin due to the effects of gravity and actinic damage. Also, with age come perioral fine lines and rhytids, mentolabial folds due to sagging of the corners of the oral commissures also known as marionette lines8, and flattening of the Cupid’s Bow and the philtral column. External factors, such as smoking and sun exposure also help accelerate the ageing process.
Aesthetics
Symmetry and proportions play an important role in defining the attractiveness of a youthful face. Over time these ideals have changed and today’s practitioner must conform to these changes to achieve the desired treatment goals. For the purpose of considering the aesthetic ideals, the face is divided into horizontal thirds. The upper third from the hairline to the glabella, the middle third from the glabella to the base of the nose, and the lower third from the base of the nose to the tip of the chin. Within the lower third, the lips must conform to the golden ratio of 1:1.618 of the upper to the lower lip to be considered aesthetically pleasing9. This ratio applies mainly during aesthetic analysis of Caucasian and European lips. In the Eastern part of the world, this ratio could even be 1:1. Additionally, laterally, the upper lip should project 1–2mm further out than the lower lip.
These ideals have evolved over time serve as a template for today’s practitioners to formulate a treatment plan.
Fillers
There is an increasing list of treatment options available in the market today for the purposes of lip augmentation. Techniques such as dermabrasion, laser, and chemical peels are commonly used for lip rejuvenation by treating the perioral area10. However, the most common approach for lip augmentation and aesthetically pleasing lips is the use of commercially available dermal fillers11.
In the beginning, bovine collagen was the soft tissue material of choice for facial rejuvenation; however, an ideal filler today is one that is biocompatible, biodegradable, adjusts easily to the patient’s anatomy, appears natural, and is not permanent. One molecule that conforms to all these properties is hyaluronic acid (HA).
Hyaluronic acid
Hyaluronic acid is a naturally occurring, highly hydrophilic polymer discovered 70 years ago. Hyaluronic acid, also known as hyaluronan, is an anionic, nonsulfated glycosaminoglycan distributed widely throughout connective, epithelial, and neural tissues. The average 70 kg (154 lb) person has roughly 15 grams of HA in their body, one-third of which is degraded and synthesized every day12. HA is a glycosaminoglycan disaccharide composed of alternately repeating units of D-glucuronic acid and N-acetyl-D-glucosamine13,14.
The hygroscopic properties of HA enable it to serve as an excellent soft tissue lip filler as it absorbs high quantities of water thereby hydrating and volumising the lips13. Another major advantage of HA is that it can be cross-linked to form gels of various thicknesses. Fillers with high cohesivity and less viscosity are softer and are subsequently chosen to be used for lip augmentation. The Juvederm Ultra XC (Allergan, Irvine, CA) was used for the purpose of this study.
Techniques
Augmenting the perioral region with injectable fillers requires skill and experience on the part of the medical practitioner especially with respect to the final position of the injected material in vivo. Additionally, the injecting plane differs with each individual’s anatomy, so no one technique can be used for all cases. However, the standardized techniques yielding good results have been reviewed in this article.
Common techniques for augmenting deep lip tissue include the spot bolus or depot technique; the linear threading and serial puncture technique is used for outlining or enhancing the upper or lower lip, while vertical linear threading is performed to enhance the philtrum and Cupid’s bow. The aim of each technique is to achieve maximum results with the least material and injury, for augmentation with a natural-looking result. It is observed that combinations of these techniques yield the best outcomes.
Study design
A 6 month prospective, open-label, multi-centre observational study of 50 subjects was performed to evaluate the aesthetic impact of treatment with hyaluronic acid for lip augmentation.
Results were evaluated by both physician and subject immediately after injection and then again after 8 weeks at the follow-up visit. The assessment of lip fullness was performed with the aid of a questionnaire completed by the subject (QS1) immediately post-injection and after 8 weeks of injection (QS2).
Key exclusion criteria included any subject with history of semi-permanent filler or permanent implants in their lips.
Results
Satisfaction with improvement in
the natural look of the lips
Satisfaction with the feel of the lips
When rating the feel of the lips as either smooth or lumpy post injection, most clients (47 of 50 subjects) rated the feel as smooth and the remaining (3 of 50) rated it as a lumpy and irregular. At the follow-up visit post 8 weeks all clients considered their lips to be smooth with no irregularity.
Comfort of injection
The subjects rated the injection following a 4 score pain scale as 0=painless, 1=slight discomfort, 2=discomfort, 3=painful, and 4=unbearable. Most subjects rated the procedure at 1=slight discomfort (38/50), a few as 0=painless (14/50), and remaining at 2=discomfort (8/50).
Hydration and improvement
in lip wrinkling
Subjects were offered four rating categories — no change, hydrated but no improvement in lines, slight improvement in lines, and significant improvement. The ratio of clients with noticeable change in hydration and wrinkles (33/50) was higher than the no change (8/50) and (9/50) slight improvement groups.
In all the cases, to ensure client comfort during the treatment, a topical anaesthetic was applied and kept on for 15 minutes. The product used was a combination of lidocaine and prilocaine.
Using a HA soft tissue filler containing lidocaine not only reduced the pain of the injection, but also reduced the client’s apprehension to the pain. Before the advent of soft tissue fillers with built-in lidocaine, dental blocks were used to reduce client discomfort. There was no bruising noticed post treatment. An ice pack was placed on the site of injection. The treatment site was cleaned and an anti-inflammatory gel was applied.
To further expand on the improvements that can be attained, individual cases are discussed below.
Case 1
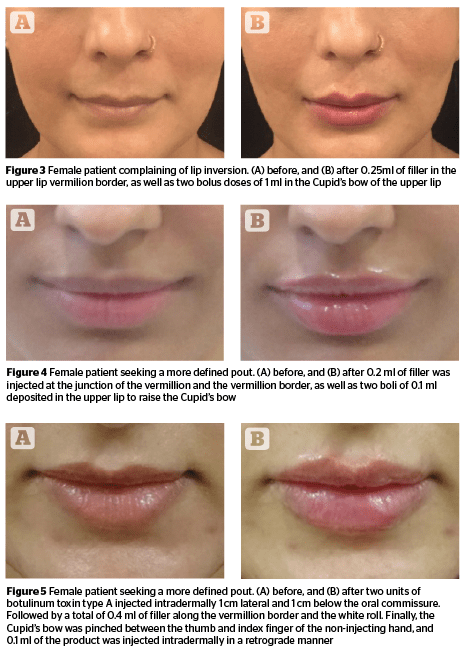
A 27 year old female, presented with a complaint of lip inversion that was more prominent when smiling.
In this case, looking at the client’s age and requirement, she was assessed from all angles. Since teeth and bones support the shape and volume of the lips, it was important to evaluate her dental frame, which showed no abnormality.
It was decided to first define her upper lip vermillion border using a threading technique. The lip was held in place by applying gentle downward force to pair the tissue against the teeth. The needle was inserted 3 mm deep and positioned from the lateral to medial segment of the upper lip vermilion border. A total of 0.25 ml of filler was injected as the needle was slowly withdrawn to implant a continuous depot of filler. The needle was then inserted 1 bevel deep at the modiolus and a bolus of 0.1 ml was deposited to add volume to the ends of the oral commissure and also lift the oral commissure as seen in Figure 3. Hyaluronic acid of 24mg/ml viscosity was selected as the product of choice; since the filler is hydrophilic by nature (i.e it absorbs water), it was best under-corrected
Case 2
A 27 year old model (Figure 4) wished for a more defined pout. Injections along the vermilion border typically enhances the projection of the lip to help create a pout. To help achieve this, a 30 G, half inch needle was used to inject the HA filler. Starting at the corner of the mouth, a linear thread of the filler was deposited along the upper lip vermilion border creating a soft projection. A sensual lip has a distinct ‘white roll’ that reflects light. Photoaging and external factors, such as smoking, leads to loss of the white roll. Exactly 0.2 ml of filler was injected at the junction of the vermillion and the vermillion border, on either side where the tissue transitions from skin colour to lip colour. To create the sensual pout it was necessary to accentuate the central portion, i.e. Cupid’s bow. Following the same protocol of cleaning and applying anaesthesia, two boli of 0.1 ml were deposited to raise mounds on the upper lip using a vertical linear thread technique; the non-dominant thumb and forefinger were used to grip the injecting lip to help guide the product into the exact location. The tip of the needle was lifted to ensure placement exactly at the peak point of the Cupid’s bow, as even a shift of 0.5 mm can change the two ‘high’ points of the Cupid’s bow.
For the lower lip, two tubercles were created by entering the lower lip at the white vermilion and depositing a bolus of 0.1 ml on each side in line with the philtral ridges.
With all of 0.8 ml of hyaluronic acid 24mg/ml, the desired pout and sensual lips were created to the subject’s satisfaction.
Case 3
A 37 year-old female subject complained of volume loss to the lips. After analysis it was noticed that other than volume loss there was also hypertrophy of the orbicularis oris resulting in inversion of the corners of the lips and volume loss (Figure 5).
After following the above mentioned protocols of cleansing and anaesthesia, the client was first treated with two units of botulinum toxin type A on each side to lift the oral commissure by addressing the depressor anguli oris muscle, injected intradermally 1 cm lateral and 1 cm below the oral commissure. One week later, the subject was treated with Ha 24 mg/ml.
The needle was inserted 1 bevel deep beginning 1 cm away from the corner of the mouth. The material was injected using a linear threading technique along the vermillion border and the white roll; a total of 0.4 ml was used to segment the upper lip. The philtral ridges were also defined to give the lips an uplifted, everted appearance. The Cupid’s bow was pinched between the thumb and index finger of the non-injecting hand, and 0.1 ml of the product was injected intradermally in a retrograde manner, just lateral to the imaginary line to create the philtrum.
For the lower lip, two tubercles were created by entering the lower lip at the white vermilion and depositing a bolus of 0.1 ml on each side in line with the philtral ridges. Once the tubercles were created, the dry ends were hydrated by linear threading at the submucosal level.
Case 4
A 25 year-old male model desired greater definition in his upper lip (Figure 6). Due to professional requirements the subject desired a very natural look.
On analysis it was decided to only define the upper lip border to give definition and shape to the lip. After following the above mentioned protocols of cleansing and anesthesia the patient was injected with HA 20mg/ml.
The vermillion border was enhanced using a multi puncture linear threading technique. Beginning from the corner of the mouth with needle bevel deep a thin layer of material was deposited along the length of the needle. The second puncture was made at the end of the first puncture and so-on until the entire upper lip border was completed. Total volume of 0.35 ml HA was used to yield this result.
Complications
Local injection site reactions are the most 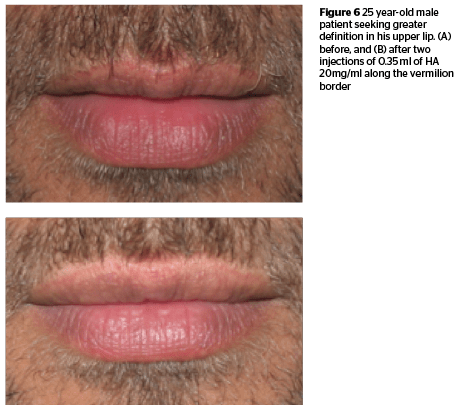
Regarding late-onset complications, the most frequent are the development of inflammatory nodules, granulomas, and sterile abscesses; the bacterial colonization of the implant can also cause a chronic inflammatory reaction around the injected area16.
Lips being a smaller area of injection, if the hayaluronic acid is injected slowly and not superficially, complications are rarely encountered. Lumps may occur that can be moulded in the first 24 hours post injection.
Conclusion
The following points succinctly summarise the key aspects to consider when performing lip rejuvenation treatments:
- The author believes in the divine ratio of 1:1.618, however, experience has taught them that Indian and South Asian patients do not favour the larger lower-lip the ratio would yield; therefore, the author works with the proportion of 1:1. To create balance, both upper as well as lower-lip correction is advised.
- It is important to consider the relationship between lip height and incisor to evaluate possible maxillary hypoplasia and protrusion, and to consider the patient’s occlusion status. This way even a small bit of filler, especially in the vermillion, will evert the lip too much with an undesirable outcome. Therefore a full facial analysis is important to ensure best results.
- Since the lip and peri-oral area are highly vascular, before injecting, it is imperative to aspirate to ensure that intravascular placement of the product does not occur
- To avoid bruising, always inject a smaller amount and inject slowly
- For novice injectors, the author would advise that if one can see the outline of the needle, it is probable that placement will be too superficial and the needle should be repositioned. If, after injecting about 0.1 ml of product, there is no visible difference in the area treated, it is possible that the needle is too deep and it should be moved more superficially
- Remember to undercorrect as hyaluronic acid used for ‘lip augmentation’ is hydrophilic in nature and the author firmly believes ‘less is more’ especially when injecting the lips.





