Non-ablative rejuvenation
The field of non-surgical skin rejuvenation continues to gain popularity as the ability to attain cosmetic enhancement with minimal risk and rapid recovery increases. Laser skin resurfacing was first introduced in the 1980s, but had a high rate of side-effects including persistent erythema, permanent hypopigmentation, scarring and a prolonged recovery time. This encouraged the development of non-ablative and fractional resurfacing to minimise risk and decrease recovery time13, 14. Although the ablative CO2 and Er:YAG lasers have remained the gold standard for resurfacing, newer systems stimulate collagen production and remodelling with little-to-no healing time and less patient discomfort15, 16. Additionally, despite the significant results seen on the face with ablative fractional devices, non-facial areas such as the neck, chest and hands are more difficult to treat owing to increased risk of prolonged healing time, scarring
and dyspigmentation17, 18.
Non-ablative resurfacing can produce minimal thermal injury to the dermis in order to improve rhytides and photodamage, while preserving the epidermis. Fractional resurfacing further increases the efficacy of non-ablative and semi-ablative procedures, but with a quicker recovery period compared with ablative resurfacing13. Thermal but non-ablative procedures involve selective thermal injury to the papillary and upper reticular dermis, where the majority of solar elastosis is located in photodamaged skin. This leads to fibroblast activation and synthesis of new collagen without epidermal damage19–25.
Intense pulsed light therapy
Short pulsed and short wavelength lasers have been replaced by longer wavelength infrared lasers that specifically target the mid-dermis and result in a more consistent, albeit milder, improvement of rhytides. Intense pulsed light (IPL) devices target both dyspigmentation and vascularity, resulting in an overall improvement of photodamage13. Lentigines, telangiectasias and epidermal pigment have been successfully treated with IPL26, 27.
The global improvement of dyspigmentation and vascularity seen with IPL (515–1200 nm) is a result of the fact that the device targets both melanin (400–755 nm) and haemoglobin (580 nm)28. Furthermore, histologic neocollagenesis, as well as an increase in extracellular matrix proteins, can be seen 6 months after treatment19, 29. The addition of 5-amminolevulinic acid (ALA) prior to an IPL treatment has shown greater pigmentary and vascular improvement, as well as a more pronounced improvement of fine rhytides following two monthly treatments30, 31.
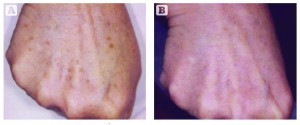
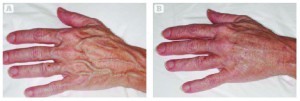
Cut-off filters are used in IPL therapy so that treatment parameters, different targets and depth of desired penetration, can be adjusted based on the patient’s skin type2, 28. In 2011, Sasaya et al32 treated solar lentigines on the dorsal hands with a 500–1200 nm non-coherent, filtered broadband pulsed flash lamp. They demonstrated a moderate to marked improvement of solar lentigines in 62% of patients and a patient satisfaction survey revealed that 65% of patients were satisfied to very satisfied with the results. The group used a 515 nm filter for shallower penetration into the dermis and higher absorption of melanin32.
Light-emitting diode therapy
Light emitting diodes (LEDs) encompass another category of non-thermal light therapy that has no reported side-effects. It has been shown to accelerate wound healing after thermal-based rejuvenation treatments with the activation of fibroblasts, as well as showing anti-inflammatory properties33–41. LED treatment can enhance the efficacy of photodynamic therapy owing to multiple wavelengths and a large, uniform beam profile, as well as reduce pain associated with the procedure39, 40. Improvement of photodamaged and aged skin can be seen with a variety of narrow-band LEDs that stimulate natural intracellular photobiochemical reactions. Additionally, non-thermal photobiological processes are responsible for accelerating wound repair38, 42–46. Multiple clinical trials using a 590 nm wavelength LED to treat photoaged skin were shown to effectively stimulate collagen synthesis, as well as reduce elastosis, erythema and pigmentation in 60–90% of patients35, 38.
Radiofrequency therapy
RF devices were developed in order to increase penetration depth and cause collagen shrinkage with skin tightening47. Traditional lasers create heat by targeting selective chromophores, while RF technology produces an electric current that generates heat through resistance in the dermis and subcutaneous tissue48–50. The tissue is heated to a temperature of 65–75°C, the critical temperature that causes denaturation and contraction of collagen and consequently, tissue tightening48, 51, 52. The energy produced by RF develops a heat that is regulated according to the tissue depth, from the superficial dermis down to the muscle border. Tissues with higher impedance, such as adipose tissue, will produce a greater heat and therefore a greater thermal effect53. Based on the principles of selective photothermolysis, the sequential exposure of these wavelengths on target tissue chromophores results in selective thermolipolysis and thermodenaturation of collagen fibres, causing enhanced skin retraction and contraction54. With the use of RF technology, shorter wavelengths are more effective at targeting pilosebaceous, vascular and pigmentary changes, while longer wavelengths are most effective in the reduction of wrinkles through dermal remodelling55.