Abstract
Throughout a person’s lifetime, the face and hands receive the most sunlight exposure, and therefore show the most photodamage in the form of dyspigmentation, texture changes, wrinkles, and loss of volume. Although current aesthetic dermatologic treatments primarily target the face, rejuvenation of the hands to treat photoageing is also an important consideration. Inherent tissue properties of the hand make it challenging to safely and effectively improve pigmentation, wrinkles and texture with a single device. Technology has evolved from painful procedures that required significant downtime to non-painful, non-invasive procedures with no downtime and effective results. Specifically, light and radiofrequency-based technologies continue to be implemented and improved on to achieve the optimum degree of photorejuvenation for the aesthetic patient.
Skin is composed of a network of collagen and elastic fibres, which determines its firmness and elasticity. As a person ages, this network loosens and begins to alter the appearance and function of the skin1. The epidermis thins and the appearance of lentigines, actinic keratoses and seborrhoeic keratoses emerge. There is an overall decrease in the quality and quantity of collagen and elastin in the dermis, as well as an increase in bruising, as a result of ultraviolet light damage to capillaries2. Approximately 1% of dermal collagen in adult skin is lost each year owing to an increase in collagen degradation and a decrease in collagen synthesis1.
There are both extrinsic and intrinsic factors involved in the ageing process of the skin. Intrinsic changes are genetically predetermined and occur as a natural result of ageing, while extrinsic factors are controllable and include sun exposure, pollution and smoking, as well as movements over time and lifestyle components like nutrition, sleep position and a patient’s overall health3.
The appearance of the hands can often reveal a person’s true age, especially if it does not correspond with a younger-looking face4, 5. The clinical manifestations of the ageing hand are based on the pathophysiology of the epidermis, dermis and subcutaneous tissues. The epidermal components present as pigmentary changes, such as lentigines and ephelides, as well as generalised hyperpigmentation. Skin roughness can occur as a result of irregular epidermal contours and abnormalities in cell proliferation and turnover. Dermal components involving structural changes in collagen, elastin and glycosaminoglycans are expressed as wrinkles. Alterations to the deeper structures, including the subcutaneous tissue, muscle and bone, may result in skin laxity, volume loss and prominent veins6.
Treatment considerations
The anatomy of the skin on the dorsal hand differs from that of facial skin and must be addressed accordingly. The dermis is thinner on the dorsum of the hand than it is on the face, and there are fewer adnexal structures, such as pilosebaceous units and superficial dermal vessels4, 7, 8. During the course of the healing process, pigmentary changes occur more frequently because the hands have less capacity to replace the epidermis2.
Clinically, the hands tend to show more significant photoageing owing to inconsistent and inadequate sunscreen use, as compared to the face9. Inherent tissue properties of the skin of the dorsal hand have made it challenging to safely and effectively improve pigmentation, wrinkles and texture with a single device10.
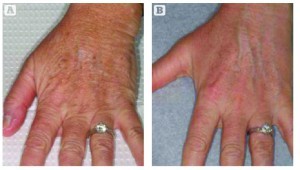
Figure 1 (A) Before and (B) after treatment with the Fraxel laser (Solta Medical, Inc., Hayward, CA, USA)
In order to objectively quantify the severity of the ageing hand, a scale for hand grading was developed. It is a five-point photonumeric scale primarily based on volume loss and the appearance of superficial veins. The scale ranges from 0, no loss of fatty tissue, to 4, very severe loss of fatty tissue and marked visibility of veins and tendons11. An algorithm was also designed by incorporating the scale, in order to formulate a treatment approach for ageing hands using combined photorejuvenation techniques. Narurkar12 suggested that patients who meet scale ‘0’ and have no loss of fatty tissue should be using sunscreen as well as topical retinoids. Those who meet scales ‘1–3’ are best treated with non-ablative fractional resurfacing and subsequent volumetric restoration with dermal fillers, with the possible addition of unipolar radiofrequency (RF). Ablative fractional resurfacing, dermal fillers and unipolar RF are recommended for scale ‘4’ patients, who exhibit severe photodamage and laxity12.




