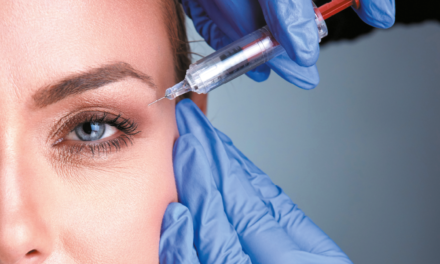
Sabine Zenker, Enrique Lorente, Fernando Galcerán, Rafaela Vidal, Ignacio Ordiz, Josefina Martinez, and Luis Luis discuss using injections of hyaluronic acid, polynucleotides, organic silicon, and DMAE to rejuvenate the skin
Skin ageing is an ongoing process, typically dividable into two mechanisms: extrinsic and intrinsic ageing. The primary trigger for skin changes from extrinsic factors is photoaging. The pathomechanism is the formation of free radicals causing oxidative damage as well as the induction of an inflammatory milieu taking place in both the epidermis and dermis. Overexpression of metalloproteinases (MMP) speeds up the ageing process through collagen degradation. The complex process results in a decrease in collagen type I and degeneration of extracellular fibres1, with atrophy in all layers, thinning of the epidermis and dermis with reduced elasticity, the formation of wrinkles and folds (solar elastosis) as well as irregular pigmentation, broken vessels, and possibly skin cancer and its precursors.
Intrinsic skin ageing is a process based on chronobiologic, genetically determined ageing influenced by hormones, such as oestrogen, responsible for skin elasticity, water retention, and circulation; androgens, which increase sebum production; and gestagens, which inhibit the enzymatic depletion of connective tissue. The reduction of hormones present in menopause results in typical skin changes, such as the reduced thickness of the epidermis, reduced proliferation activity of the keratinocytes, and a diminished capacity for differentiation. Throughout the dermis, a depletion of up to 30% of collagen fibres occurs in the first 5 years of menopause and skin matrix proteins are also reduced. The skin gets rough, wrinkly, more sensitive, more easily vulnerable, and benign lesions such as seborrheic keratosis can occur.
So, summarizing the structural and functional changes occurring at the epidermis and dermis during the ageing process, one can see again alterations in dermal collagen, elastin and glycosaminoglycans1; a loss in the content of hyaluronic acid resulting in skin dehydration and loss of turgidity with overall thinning; and loss of elasticity and impaired response to ultraviolet light2,3.
Mesotherapy
Mesotherapy to treat aged skin works through multiple micro-dosed superficial injections using specific injection techniques, such as epidermal-nappage, micro-papular or the point-by-point technique to inject bioactive substances in the skin to treat cosmetic conditions4. The therapeutic aim of mesotherapy for skin rejuvenation is to increase the activity of the fibroblasts by inducing an optimal physiologic environment to enhance the cell activity and, therefore, encourage the synthesis of collagen, elastin, and hyaluronic acid.

Figure 1 In vitro study fibroblasts/polynucleotides. Twenty-four hours after treatment with HA, normal dermal cell regeneration capacity increases by 96%. Assessment of dermal regeneration capacity (fibroblast proliferation and migration) in base culture medium (Control) (A) or base culture medium supplemented with HA (B). Images captured at 0h and after 24h with the optical microscope. Source: Biotechnology Unit. mesoestetic Pharma Group S.L. 2016. Product used: mesohyal™ Hyaluronic
The desired clinical result is firm, bright, and moisturised skin. Typically, a liquid mixture of compounds such as hyaluronic acid, pharmaceutical and homoeopathic medications, plant extracts, vitamins and other ingredients, such as platelet-rich plasma is used to improve the overall quality of the skin. Hyaluronic acid especially has proven to increase the skin’s elasticity, hydration, and firmness4.
In vitro data
It is well known that injection of non-reticulated hyaluronic acid (HA) attracts water molecules, therefore hydrating the tissue and stimulating collagen synthesis. Hyaluronic acid is also involved in other processes, such as wound healing, neutralisation of free radicals, and it interacts with proteoglycans in the extracellular matrix5,6.

Figure 3 (A) before (B) after treatment of a 49 year old female patient with 2.5 ml mesohyal™ X-DNA + 2.5 mesohyal™ DMAE
Dimethylethanolamine (DMAE) is a precursor of acetylcholine, a neurotransmitter that intervenes in muscle contraction. It increases epidermal and dermal thickness, enhances stratum corneum water content and inhibits the formation of lipofuscin (pigment)7–12.
Recent studies show that mesotherapy by injecting DMAE combined with amino acids (AA) can regulate the collagen catabolism resulting in collagen stimulation13. Other studies show a decrease in the production of collagen type I and an increase of collagen type III and MMP-1 in ageing skin treated likewise14. Results obtained from these studies indicate that mRNA expression for collagen type III and MMP-1 is much less in ageing cells than that of normal tissue14. It might be that collagen metabolism undergoes a different process between regular skin changes with ageing and a D-galactose-induced subacute skin ageing model14. According to this study, injection of DMAE or AA alone showed no effects on hydroxyproline content or messages for type I collagen and MMP-1 in ageing skin. These data indicate that the concomitant use of DMAE and AA might be the only way to exert their antiageing action in this D-gal induced ageing skin model, by modulating collagen type I metabolism and remoulding the structure of the ageing skin14.
Organic silicon
Organic silicon, an element the skin is rich in, acts at a structural level ensuring the integrity, tone, and elasticity of cutaneous tissue and binds to collagen, elastin, and proteoglycans. The reserves of silicon deplete progressively with age. However, a silicon supplement can improve skin hydration and tone, resulting in firmer, softer skin with a greater repair capacity. Indexed studies report that fibroblast culture irradiated with UV-A rays to simulate photoaging produce less collagen and present less resistance to traction (less elasticity). Thus, organic silicon has the potential to stimulate fibroblasts to synthesise collagen and to increase skin elasticity15, 16.

Figure 4 (A) before (B) after treatment of a 44 year old female patient with 2.5 ml mesohyal™ Hyaluronic + 2.5 mesohyal™ Organic Silicon
Polynucleotides (PN) are biopolymers composed by nucleotide monomers DNA (deoxyribonucleic acid), and RNA (ribonucleic acid) are examples of PN. Polynucleotides have shown to improve tissue regeneration17–19. On the one hand, nucleotides are composed of a nitrogenous base, a pentose sugar and phosphoric acid. On the other hand, polynucleotides are organic compounds formed by covalent bonds between nucleotides.
The diagram shown in Figures 1–2 highlights the results of an in vitro trial to improve cell regeneration of human fibroblasts by adding non-reticulated hyaluronic acid (HA) to the cell culture.

Figure 5 (A) before (B) after treatment of a 49 year old female patient with 2.5 ml mesohyal™ X-DNA + 2.5 mesohyal™ DMAE
Twenty-four hours post treatment the fibroblasts showed an increased dermal cell regeneration capacity by 96%.
Twenty-four hours post-treatment with HA, the fibroblasts showed an increased collagen synthesis capacity by 92%. When polynucleotides were added to the culture medium, an increase in the number of fibroblasts and the synthesis of extracellular matrix proteins (collagen, elastin and fibronectin) was recorded.
Other studies proved the synthesis of growth factors (EGF, FGF, etc.)20 and enhanced cell protection against solar radiation21.
In vivo data
Material and methods
A prospective study was performed with twenty Caucasian women aged 41 to 69 years, with a Glogau score of 2 or higher. Volunteers were divided into two subgroups: Subgroup A — those experiencing dehydration and loss of elasticity, and Subgroup B — those women experiencing sagging. All subjects received five mesotherapy treatment sessions for facial skin ageing using either organic silicon and sodium hyaluronate (concentration of 2.5 mg/ml) or polynucleotides, dimethylaminoethanol, and sodium hyaluronate (2.5 mg/ml), respectively. Injections were performed intradermally. Efficacy was evaluated objectively by the cutometer for elasticity (Subgroup A) and firmness (Subgroup B). The corneometer evaluated hydration levels. Safety was assessed for each treatment session.

Figure 6 (A) before (B) after treatment of a 51 year old female patient with 2.5 ml mesohyal™
Hyaluronic + 2.5 mesohyal™ Organic Silicon
Subgroup A included individuals with signs of dehydration and loss of elasticity. Their treatment was based on mesohyal™ Hyaluronic + mesohyal™ Organic Silicon.
Subgroup B included individuals who had marked flaccidity. The treatment was based on mesohyal™ X-DNA + mesohyal™ DMAE. Treatment was applied in five sessions at intervals of 15 days between each visit. In both groups the facial administration protocol was the same.
Technique
Mesotherapy-wise intradermal injections to the skin of the face to the epidermis and superficial dermis, approximate injection depth 3 mm, the approximate amount of product is 0.05ml/ppt using a 1–3 ml Luer-lock syringe with a 4 mm 30G sharp needle. The total volume of product injected per session was approximately 3–5 ml/session; 5 treatments in total.
Evaluation of efficacy was completed at two follow-up visits (after 3 sessions and one week after the end of treatment) using a Cutometer™ probe (Courage – Khazaka Electronic) for skin elasticity measurements in Subgroup A and firmness evaluation in Subgroup B. Additionally, a self-assessment was performed by each patient after completion of the study.
Safety assessment evaluated both immediately after each session and 15 days after each session with no unexpected side-effects or adverse events reported.
Results
The results in Subgroup A (hyaluronic acid + organic silicon) showed that skin elasticity improved up to 19.4%, while with Subgroup B firmness improved up to 25.4%. In both subgroups, a noticeable improvement was observed in assessing the fine wrinkles and skin hydration in over 85% of the volunteers. As per the self-assessment, 90% of the volunteers reported a noticeable improvement in the hydration of their facial skin after five sessions.
In Subgroup B (polynucleotides + DMAE + sodium hyaluronate) 80% of the volunteers reported a noticeable improvement in skin hydration after 5 months of treatment.
The intradermal administration of mesohyal™ X-DNA and mesohyal™ DMAE showed an improvement in skin elasticity of 19.35% after five sessions of treatment, according to objective data obtained from the Cutometer™.
Conclusion
Typical signs of skin ageing are dehydration and its loss of elasticity and firmness. This study data evaluates changes in skin elasticity, firmness, and hydration after intradermal injection of different actives such as non-reticulated hyaluronic acid, polynucleotides, organic silicon, and dimethylethanolamine to the facial skin as well as the treatment’s safety and efficacy. Both combined mesotherapy protocols proved to be an effective and safe tool to improve the overall skin quality suited to treat ageing facial skin.