Materials and methods
A systematic literature search was conducted of the following electronic databases: Medline, Scopus and PubMed. The key words used for the online research were a combination of: ‘rhinophyma treatment’, ‘rhinophyma surgery’, ‘severe rhinophyma’, and ‘rhinophyma management’. After the first step of the selection process, the retrieved articles were fully analysed. Articles without available full-text or with excessive missing data were excluded. All relevant articles were then reviewed for the author name(s), the publication year, the treatment option used, and the number of cases reviewed.
If details of the procedure were unclear, the article was excluded. All of the previous data were considered important to properly investigate which techniques are currently used for the treatment of rhinophyma and which was the safest and most appropriate in cases of severe rhinophyma.
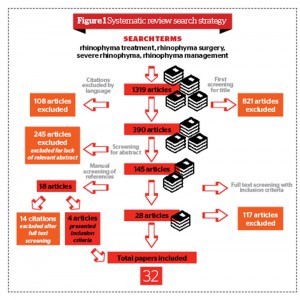
A flowchart of the systematic article selection and evaluation is illustrated in Figure 1.
Results
Of the initial 1319 studies yielded from the search (Figure 1), 390 studies qualified for the second stage of selection, and after the screening of 145 full-text papers, 55 studies met the definitive inclusion criteria. Of the selected 55 articles, 32 were case series, original papers or retrospective reviews and were included, while 13 were case report papers and therefore excluded. A spectrum of surgical options is currently available, but no universal agreement exists as to which treatment method delivers the best results; furthermore, no single method seems to be free of complications and all carry a degree of morbidity16. The described techniques include total excision with subsequent skin grafting or flap cover, and partial excision (or ‘decortication’) with the cold scalpel, Shaw knife (Hemostatix™ Medical Technologies, Bartlett, TN), electrocautery, cryotherapy, chemical peel, dermabrasion, dermaplaning with a dermatome, ultrasonic scalpels, laser excision (CO2 laser and argon laser)16,19, and VersajetTM Hydrosurgery System20 (HydroCision Inc., North Billerica, MA).
Discussion
Aetiology and classification
Rhinophyma, a benign disfiguring disease affecting the nose, is a rare condition caused by a progressive hypertrophy of sebaceous glandular tissue, connective tissue, and blood vessels. The condition affects mainly the lower half of the nose and results in a tuberous appearance leading to cosmetic disfigurement and occasional functional problems. The deformity may be localised or generalised and is often the cause of cosmetic embarrassment and social reclusion. When left untreated, the nose can reach giant proportions over the years.
The aetiopathogenesis of rhinophyma remains unclear; Marks21 proposes a mechanism for rhinophyma evolution that begins with vascular dysfunction in the skin. Indeed, the skin in rosacea is characterised by an unusual disorganisation of the upper dermis, resulting in an instability of the superficial cutaneous vascular plexus. Consequently, any vasodilating agent (such as alcohol, spicy foods, and hot beverages.) may cause loss of intravascular fluid with oedema of surrounding tissue. This oedema may disappear slowly in the nose and fibrosis may occur, causing the nose to gradually enlarge22.
Histopathologically, two forms of rhinophyma were described by Tope and Sangueza23. The most common is characterised by histological lesions that are peculiar of rosacea, such as hyperplasia of sebaceous glands, dermal elastosis, follicular cysts, and moderate fibrousness with collagen fibres plunged in a myxoid or oedematous stroma. A perifollicular infiltrate composed of lymphocytes, histiocytes, and plasmocytes is also prominent in the dermis. The second form or ‘fibrous variant’ shows severe fibrotic alterations in the dermis with thickening, through which dilated capillary and lymphatic vessels are found; a decrease or lack of sebaceous glands; and dermal annexes23, 24.
A number of clinical classifications of rhinophyma based on severity of deformity have been proposed25,26. El-Azhary et al26 classified the rhinophyma in low, moderate, and severe stages of disease. With this model it is possible to find telangiectasia and low hypertrophy of the cutaneous layer in the first case, moderate hypertrophy and small nodularities in the second case, and massive nodularity in the severe form.