Sabine Zenker presents her concept for the treatment of wrinkles and midface volume loss with hyaluronic acid and polycaprolactone.
Skin ageing is a continuously and onwardly marching process typically dividable into two mechanisms — extrinsic and intrinsic ageing. Photoaging is the major trigger for skin changes from extrinsic factors1,2. The predominant pathomechanism is the formation of free radicals causing oxidative damage and induction of an inflammatory milieu3 mainly occurring in the dermis. All this results in a decrease in collagen type I and degeneration of extracellular fibres4. Clinically speaking, the skin undergoes atrophy in all layers, becomes thinner5, less elastic, and presents with wrinkles and folds (solar elastosis) as well as irregular pigmentation, broken vessels, and possibly skin cancer and its precursors.
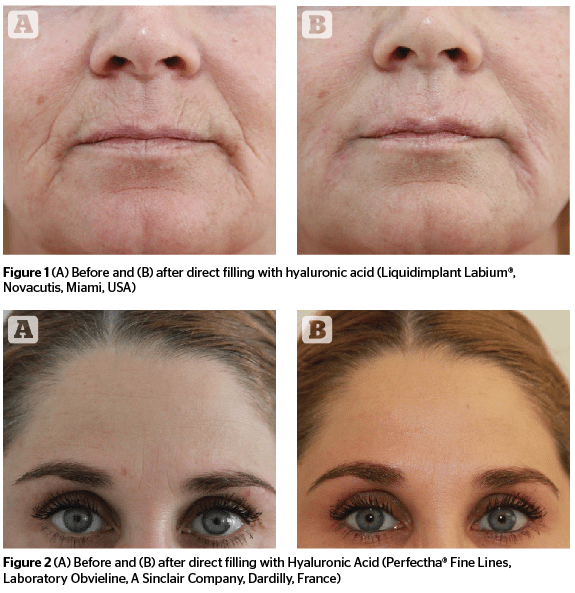
Focussing on the ageing of the facial skin, its implications for aesthetics, wrinkles, and creases in the perioral region distort and alter perceptions in a very prominent way as they are real age giveaways, and they — with the passing of the years — give facial expressions an older-looking and possibly negative aspect.
Age-related three-dimensional facial changes
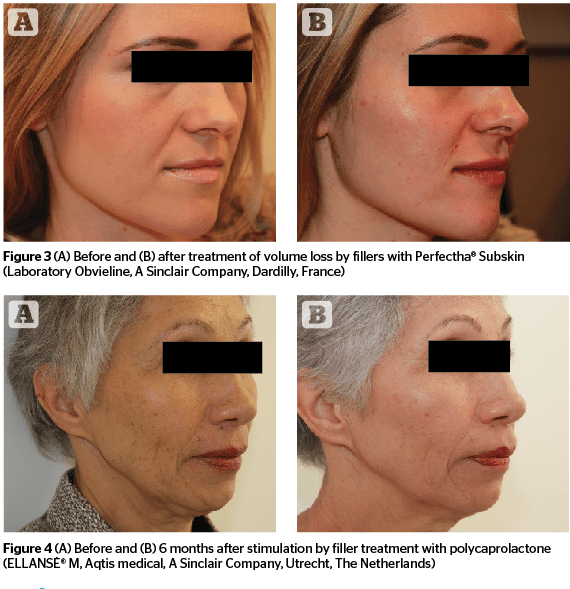
Typical indications for filler treatments
Here, very importantly, filler treatments come into play. Any treatment in dermatology and aesthetic dermatology requires an indication-specific treatment approach: before any treatment, the individual diagnosis has to be made. Typical indications for filler treatments are:
- Wrinkles: creases, folds, and wrinkles are an increasing concern, especially as we get older and they become more prominent
- Volume loss: further unwanted changes to facial features, such as the occurrence of shades, furrows, and overall sagging, are the reason patients seek help: to restore facial proportions to get back features they had in the past or to improve anatomical aspects of their face; basically, it’s about giving back a healthy look with natural fullness and soft, smooth transitions as well as erasing unwanted shades.
Technique for treating wrinkles with filler
Intradermal retrograde placement (‘blanching’) by serial-puncture or the linear-threading-technique using a sharp needle (30G ½” as well as a 31G 4 and 8 mm) are the common ways to inject filler in facial wrinkles25. The author does mix the hyaluronic acid with local anaesthetics in a ratio up to 30% (off-label-use), to achieve an optimal integration of the material in the superficial dermis. But each fold shouldn’t be corrected up to the clinical endpoint. For the author, a controlled filling using an injection system is key, as this increases the accuracy of filler placement and does reduce side-effects, such as pain and bruising, which improves the overall aesthetic outcome especially in very superficial injections26. The result of this direct filling technique with hyaluronic acid lasts— depending on material used and individual conditions — for some months.
The stimulation technique using polycaprolactone (PCL) is especially suited if an immediate filling is desired as well as a sustainable level of collagen stimulation starting approximately 3 months after injection27-28. Polycaprolactone is a biodegradable filler material consisting of microparticles of PCL suspended in a gel carrier (carboxy-methyl-cellulose (CMC)). The material is placed using a 25G 1½” blunt tipped cannula in the subdermal level, using a fan pattern in a retrograde fashion covering the whole to be treated area; the point of insertion is chosen in a 90° angle in the middle of the fold. The approximate amount of filler injected is 0.1cc.
Technique for treating volume loss with filler
To treat volume loss with filler, typically highly visco-elastic hyaluronic acid fillers with a good volumizing capacity29,30, or calcium hydroxylapatite (CaHA)31,32 for precise shaping, or polycaprolactone for sustained collagen stimulation and volume enhancement, should be used. The use of blunt tipped cannulas results in a more atraumatic31, and quicker treatment procedure, especially when the filler needs to be placed over ‘longer distances’32–37. For the two indications mentioned above, blunt tipped 25G 1½” cannulas are very suited.
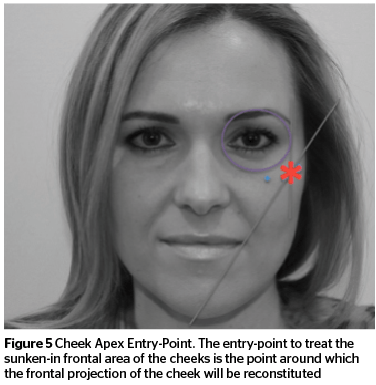
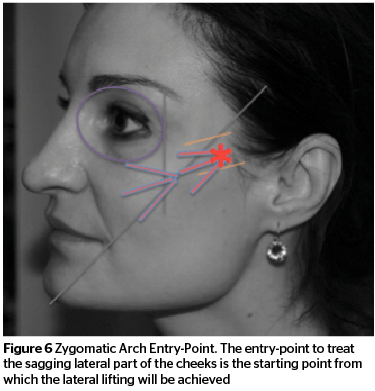
Figures 5–6 illustrate the typical entry points for this treatment concept, the cheek-apex-entry-point and the zygomatic entry-point to treat the upper-part of the midface.
The filler material used to showcase the author’s techniques here are the hyaluronic acid Perfectha© Subskin (Laboratory Obvieline, A Sinclair Company, Dardilly, France). As equipment, a blunt tip cannula 25G/38 mm is used (Steriglide®, TSK Laboratory, Oisterwijk, Netherlands).
Sunken-in frontal cheek
The starting point is the cheek apex entry-point. The filler is injected in a bolus technique (‘gunshot-wise’), in a retrograde fashion and placed supraperiostally; according to the clinical needs, more injections medial and eventually lateral of the first entry-point are performed in a ‘banana-wise’ fashion. The amount of filler per point is approximately 0.1 cc. Augmentation is conducted up to the clinical endpoint.
Sagging lateral cheek
The starting point is the zygomatic arch entry-point. The filler is injected using a fanning technique in a retrograde fashion starting supraperiostally and ending up subdermally on the most lateral part of the injection area. Amount of filler per point is approximately 0.1–0.2 cc. Augmentation is conducted up to the clinical endpoint.
Using these two techniques, the frontal projection of the cheeks can be treated and lateral lifting acheived in a customized and individual way.
Summary
Age related changes, such as wrinkles and volume loss can be easily and individually treated with filler. An indication-specific filler treatment approach shows how versatile fillers are: by applying the appropriate technique, they can be used for specific, delicate indications by precisely and elegantly filling even the smallest lines and wrinkles.