ABSTRACT
Recently, trends in aesthetic medicine have returned to easy-to-perform, effective and low-cost procedures. Electrical microneedling is one of these techniques. This article discusses the development of microneedling, its mechanism of action, and therapeutic role in the treatment of scars and ageing skin. Microneedling involves the production of thousands of controlled microscopic needle incisions in the papillary and reticular dermis. Using specially designed and manufactured sterile medical devices, the goal is to provide a physical mechanical stimulation of the dermis, while leaving the epidermis intact. This stimulates a wo=und healing repair and regeneration mechanism that results in dermal regeneration, normalised ‘basket weave’ collagen formation, and increased angiogenesis. Clinical studies have provided an objective evidence base for the efficacy and safety profile of the procedure with regard to acne scars, and texture, tone, line, wrinkle and laxity improvement in ageing and photodamaged skin. However, patient discomfort and the inflexibility of most manual skin-needling devices can be limiting factors for the intensity of the treatment and therefore, clinical outcomes achieved. This is where electrical microneedling devices come into their own, as they provide an increased level of intensity, control and comfort. The effectiveness and excellent safety profile of electrical microneedling treatments have resulted in the technique rapidly becoming established in Europe and Asia as a frontline medical aesthetic treatment for scar treatment and skin rejuvenation.
The history of using micro-incisions to improve the texture of the skin can be traced back to acupuncture, which has its roots in Chinese medicine where it has been performed for centuries. This was followed by nappage, a French skin rejuvenation technique, which can be used to replace depleted cellular levels, and in the early 1990s, subcision became popular to elevate
scars, wrinkles and lip lines1. Some years later, Camirand et al2 observed texture improvement and stimulation of melanogenesis after tattooing, with and without pigments.
Microneedling involves the production of thousands of controlled micro-incisions to the papillary and reticular dermis. Using specially designed and manufactured sterile medical devices, the goal is to provide a physical mechanical stimulation of the dermis, while leaving the epidermis intact. This stimulates a wound healing repair and regeneration mechanism that results in dermal regeneration, normalised ‘basket weave’ formation of collagen fibres, and increased angiogenesis2–4.
The effectiveness and excellent safety profile of the treatments have resulted in the technique rapidly becoming established in Europe and Asia as a frontline medical aesthetic treatment for acne scars, texture, tone, lines and wrinkles, and laxity improvement in ageing and photodamaged skin, and more recently, for stretch marks2–4.
Automated microneedling
Microneedling is not a new procedure, but is a clinically-proven and well-recognised aesthetic treatment for ageing, photodamaged skin and scar tissue. Although microneedling is not a new technique, there have been a number of refinements over the last few years. From manual devices, the trend is now moving towards automated devices, particularly as there are some limitations with manual devices, including a fixed needle length, moderate to high patient discomfort, and the widespread availability of low quality and low cost devices.
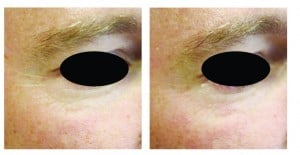
Figure 1 Male patient, aged 40 years, (A) before treatment and (B) 1 month post-treatment. The treatment was carried out using the Revive mn (amiea med, MT.DERM GmbH, Berlin, Germany), Revive-HAP, 6-point needle plate
As a result of these limitations, automated devices have been developed. This shift enables the practitioner to adjust both the speed and the depth of the needles throughout the treatments, as well as providing higher levels of patient comfort. Parameters such as needle length and the speed of needle movement can also be pre-set; therefore, penetration depth is controllable, which helps to reduce levels of pain associated with the procedure, for example.
It is important to monitor the precision and power of the automated needling devices, as these features are paramount for the strength to penetrate into the dermis with minimal trauma, and they may vary from system to system. Additionally, and of further advantage, are features such as the tilting needle plates to ensure a perpendicular incision and a reservoir to bring substances directly into the dermis. In some electrical microneedling devices, the needle plate — owing to its construction with the capability of tilting — can be adapted to fit uneven skin surfaces, or to fit the irregularities to be treated. As such, the process of needle penetration is controllable and perpendicular.
Mechanism of action
The mechanism of action of microneedling is the controlled mechanical stimulation of the wound healing response with rapid closure of the micro-incisions. The wound healing response is the result of mechanical stimulation of the dermis, which leads to higher concentrations of platelet growth factors and enhanced fibroblast infiltration. As the wound closes quickly, the need for fibrosis is minimised and the safety profile enhanced.
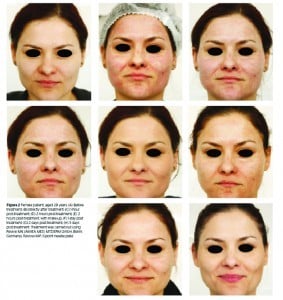
Figure 2 Female patient, aged 28 years. (A) Before treatment; (B) directly after treatment; (C) 1-hour post-treatment; (D) 2 hours post-treatment; (E) 2 hours post-treatment, with make-up; (F) 1-day post treatment; (G) 2 days post-treatment; (H) 3 days post-treatment. Treatment was carried out using Revive mn (amiea med, MT.DERM GmbH, Berlin, Germany), Revive-HAP, 6-point needle plate
In particular, microneedling leads to the gene expression of a number growth factors, collagen type I and glycosaminoglycan (GAG). The treatment leads to an up-regulation of transforming growth factor (TGF)-b1 and TGF-b2 at 2 and 4 weeks after the treatment, followed by a strong down-regulation at 8 weeks post-treatment. This triggers the natural healing process through the up-regulation of TGF-β35; up-regulation of collagen I, GAG, and growth factors6; and up-regulation of positive genes important for the epidermal–dermal junction7. This leads to normally-woven collagen and scarless healing.However, there is also a strong up-regulation of TGF-β3 2 weeks post-procedure, without any down-regulation at 4 or 8 weeks. Compared with TGF-β1 and TGF-β2, TFG-β3 is regulated highly beyond the initial phase, which supports scarless healing and a normalised collagen structure5, 8.
Further important effects of microneedling are fibroblast proliferation and collagen actuation, fibronectin and extracellular matrix deposition, re-epithelialisation and angiogenesis. Collagen matures and remodels, and leads to a tightening of the skin. This enhanced skin architecture results in an improved appearance of the skin. A notable increase in collagen and elastin fibres can be proven 6 months after a microneedling treatment1, 4. Compared with scar tissue, the collagen in the treated area is cross-linked and the stratum corneum is structured normally. Furthermore, a thickening of the epidermis by approximately 40% can be observed4.
The micro-incisions created during microneedling will close approximately 10–15 minutes after the treatment, resulting in a low risk of infection9, 10.
Microneedling offers a treatment to improve skin appearance and quality, without initiating scar formation. Owing to the low risk of post-inflammatory hyperpigmentation (PIH) compared with other methods of skin rejuvenation (e.g. laser, chemical peeling), microneedling can be used for all patients, independent of skin type and colour11. As there is no heat (compared with laser devices), this is most likely why there is limited inflammation leading to PIH.
The fact that microneedling may have a reduced risk of PIH has been discussed by Aust et al8. In their study, the authors reported that percutaneous collagen induction therapy left the epidermis intact without any damage to the stratum corneum, any other layers of the epidermis, or the basal membrane8. No signs of dermabrasive reduction of epidermal thickness were evident 24 hours after the procedure. DNA microarray experiments demonstrated that interleukin-10 was increased in percutaneous collagen induction therapy-treated skin after 2 weeks. With regard to the melanocyte-stimulating hormone gene, gene expression microarray analysis indicated a faint down-regulation both 24 hours and 2 weeks after treatment.
Enhanced substance penetration
Most molecules, like hyaluronic acid, are too large to pass the epidermis alone. However, if these substances are applied to the skin or filled into the cartridge of an automated microneedling device before the procedure, the penetration capacity and depth is more effective than that of needles alone. Indeed, skin penetration (stratum corneum) by microchanneling can result in the delivery of hydrophilic (e.g. flufenamic acid) and lipophilic (e.g. retinol) substances, and macromolecules (e.g. insulin, ALA)12–15. A needle length of 150 µm is sufficient16.The depth generally depends on the depth of needle penetration, but this is mainly into the dermis. This means that the absorption of the substance would be almost uniform throughout the area of dermis treated. The distribution outside the needle incisions may be because it is carried in lymphatic channels by mechanical force, once the molecule hits such a channel, and that this distribution is the reason for the even effect. Furthermore, hyaluronic acid provides an immediate volumising effect, which increases patient acceptance, and microneedling stimulates collagen production for a longer-lasting effect17.
Conclusions
As a result of its well-researched and proven mechanism of action, its simplicity, safety profile, and efficacy, microneedling has experienced a ‘revival’ in recent years. However, in order to match expectations such as efficacy and precision, as well as better comfort for patients, we are moving to a modern era of microneedling: automated microneedling.



