Ayda AlHammadi and Firas Al-Niaimi review the literature on the use of platelet-rich plasma to treat hair loss and androgenic alopecia.
Platelet-rich plasma (PRP) is an autologous concentration of platelets in plasma and has long been a topic of interest in vascular and orthopaedic medicine, where it aided in wound healing and tissue repair, especially in tendons, ligaments and muscles1. Although unlicensed, PRP is used in additional clinical settings since platelets are considered to be a rich source of growth factors and other beneficial cytokines1,2. In recent years, the topic of PRP has gained the attention of dermatologists due to its ability to rejuvenate hair and skin tissue. Concerning hair, PRP has shown positive outcomes in many clinical trials where it was observed to reverse hair loss, promote hair growth and enhance hair thickness1. This article reviews the current up-to-date literature of PRP and hair rejuvenation in the last 5 years.
What is PRP?
PRP is defined as a fraction of plasma from an autologous blood sample with a high platelet concentration, usually greater than 1,000,000 platelets/uL1. Upon activation, platelets release clotting factors (such as fibrinogen, von Willebrand factor, factor V), chemokines (such as Interleukin-8, beta-thromboglobulin, neutrophil activating protein, platelet factor 4), adhesion molecules (such as P-selectin) and growth factors (such as platelet-derived growth factor, transforming growth factor (beta), vascular endothelial growth factor, stromal derived growth factor 1 (CXCL 12), epidermal growth factor, fibroblast growth factor 7, b-catenin)2. The presence of insulin-like growth factor in platelets remains controversial3. The clinical effects of PRP are based on the role these released molecules achieve in the induction of inflammation, cell proliferation, differentiation, and angiogenesis2,3.
Preparation and administration
PRP preparation starts with extracting venous blood from the patient with platelet concentration being achieved subsequently through cell separation (apheresis) or centrifugation3.
The cell separation method requires a large, complex system and is usually performed by blood banks or hospitals4. However, this method is not frequently used because it is expensive, requires a large volume of blood and can cause damaged platelets4.
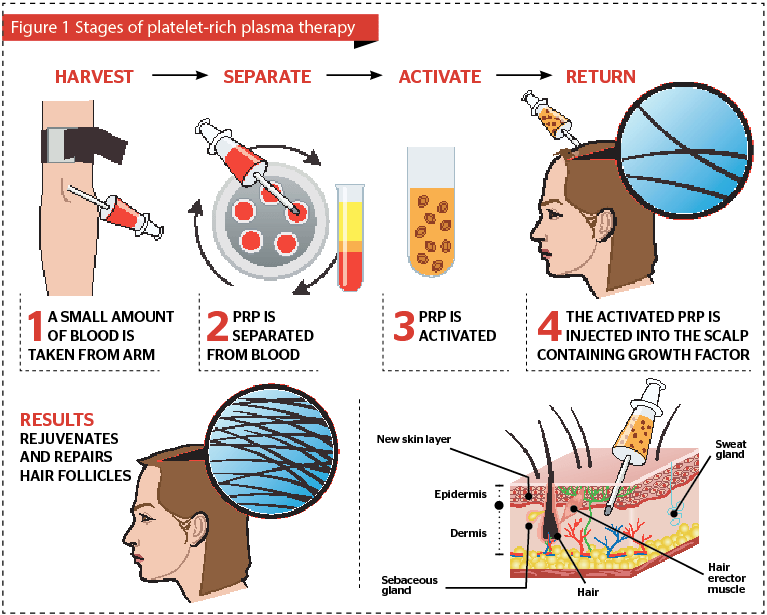
The release of growth factors starts within 10 minutes of platelet activation and more than 95% of secretion is completed within an hour of activation5. As a result, PRP should be injected within 10 minutes of activation for optimum results5. Many techniques have been used (for example, subcutaneous injections, intradermal injections, microneedling, interfollicular injections, nappage technique). The nappage technique involves giving the PRP in the form of multiple small injections in a linear pattern, usually 1-cm apart1,6. The solution can be delivered through a 1 mm insulin syringe (Leur-lock syringe) in a 27 or 30 gauge needle1,6. The procedure is generally safe, tolerable and can result in only mild irritation afterwards5. No serious allergic reactions have been reported in the literature concerning the administration of PRP for hair rejuvenation in the last 5 years.
Hair loss (alopecia)
Thick, healthy hair can signify attractiveness, youth, health, and fertility in adults and is therefore not surprising that hair loss can lead to psychological distress and low self-esteem. Unfortunately, hair loss is a common presenting complaint encountered by physicians from their patients and most fear the progression to irreversible or complete hair loss.
As a result, a detailed assessment of the patient’s history, scalp, and hair examination, together with some laboratory blood tests are required to establish the cause. Prompt diagnosis and management are sometimes needed to prevent conditions that can cause permanent hair loss7.
The hair is constantly undergoing growth cycles of different phases. These include the growth phase (anagen), regression phase (catagen), resting phase (telogen), and shedding phase (exogen)7. Each hair is completely independent of its neighbour and thus different hairs can go through different cycle phases at the same time. Accordingly, hair loss can be classified into causes that are related to problems with the hair growth cycle phases (e.g. telogen effluvium, anagen effluvium) or due to inflammation involving the hair follicle (e.g. alopecia areata, scarring alopecias)7. The hairs can be directly affected due to pathologies involving the hair follicles themselves or indirectly as a result of a wider inflammatory process involving the whole scalp skin7. Inflammatory or autoimmune conditions might need treatment with intralesional steroids, systemic steroid, immunosuppressive agents, anti-malarials or other drugs. Delay in treating inflammatory conditions can result in irreversible damage, hence it is important to understand the basic concepts of hair pathologies to halt the progression of irreversible or unnecessary h
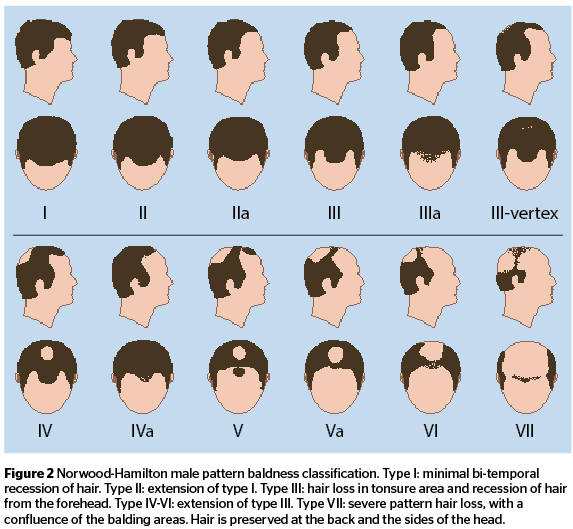
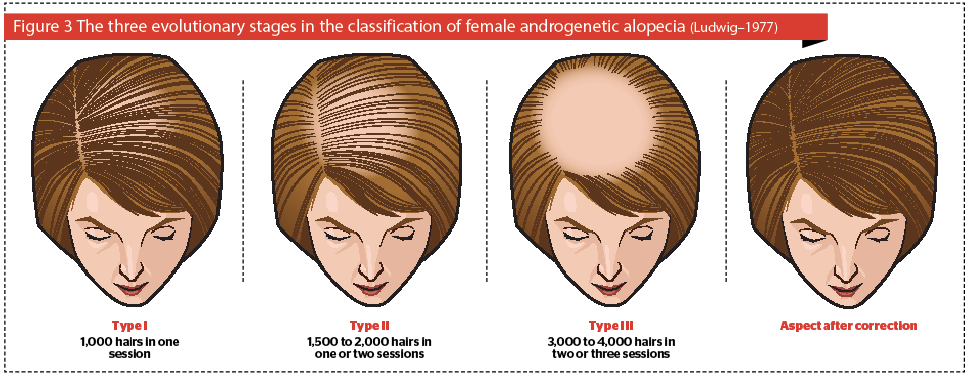
Worldwide, the most common contributing factor to hair loss is the so-called female or male pattern hair loss (FPHR or MPHR), namely androgenic alopecia. Unfortunately, androgenic alopecia affects up to 40% of women and 80% of men and the licensed treatments are only partially effective8. FPHR is characterized by preservation of the hairline and occipital scalp hair with progressive thinning of the crown and mid frontal scalp hair. MPHR classically affects the crown and temples, and may progress to complete baldness. The only licensed treatments for MPHR are minoxidil and finasteride7. Minoxidil is also licensed for FPHR but finasteride is not. However, for FPHR, finasteride and some other anti-androgens (for example, spironolactone) can be used off-licensed in women with abnormal androgens (for example, women with male pattern hair loss, acne, hirsutism, congenital adrenal hyperplasia)7. Treatments can be used alone or in combination7,8.
As this is the era of regenerative medicine and new hair therapies are emerging everyday, PRP is being studied as a treatment for hair loss. Although the study of PRP for hair loss and hair rejuvenation is still at its infancy, so far the results are promising. The procedure is regarded as safe, quick, and tolerable by most patients. Additionally, it is minimally invasive and relatively cost effective when compared to other solutions like follicular unit transplant. In fact, some studies showed that pre-treatment of follicular units with PRP, by imbedding hair follicular units in PRP solution, yielded better graft survival1,8.
Mechanism of PRP in hair loss
As mentioned earlier, when activated, platelets release many molecules including growth factors that can play a role in cell proliferation, regeneration, and angiogenesis8. It is proposed in various studies that these growth factors can act on the stem cells in the bulge area of hair follicles promoting the development of new follicles and enhancing neovascularization8,9.
Two cell types are found in this region:
- Stem cells of ectodermal origin located at the bulge area of the hair follicles, which give rise to epidermal cells and sebaceous glands
- Germinative cells of mesenchymal origin found at the dermal papilla8.
Interaction between these two cell populations in addition to interaction with the different growth factors released from platelets are believed to activate the proliferative phase of the hair and consequently give rise to a new follicular unit8–10.
The proliferation of the dermal papillae is achieved by up-regulating fibroblast growth factor-7, beta-catenin, extracellular signal-related kinase (ERK), and Akt signaling8. Vascular endothelial growth factor helps with anagen-associated angiogenesis and influences the growth of both healthy and pathological dermal structures8. The hair follicle mesenchyme displays hair-cycle associated plasticity, which contributes to the transformation of the hair follicle (e.g. vellus to terminal and vice versa like in androgenic alopecia)8–10. Modulation of this is important to reverse hair loss associated with androgenic alopecia9. PRP also improves blood supply to the hair follicles and it was observed that vascular structures have increased around hair follicles treated with PRP8–10.
In summary, the growth factors released from activated platelets promote proliferation, differentiation, and angiogenesis of hair follicles. In addition, they improve vascularization and blood supply around the follicular units. PRP also prolongs the anagen-phase and has anti-apoptotic properties9.
PRP has proven effective in pattern hair loss and androgenetic alopecia (AA)8–9. One study compared PRP injections to intralesional triamcinolone (TrA) injections in 45 patients with AA. A total of three treatments were given at a monthly interval. The study concluded that the effects of PRP exceeded those of the TrA injections, and at 12 months, 60% of the patients who received PRP showed complete remission compared to only 27% of patients who received TrA10. At 6 and 12 months, 38% and 71% of TrA patient group experienced relapse of the disease, respectively8,11. In the PRP group, the figures were 0 and 31% relapses at 6 and 12 months, respectively8,11. Moreover, only 25% of the TrA patient group experienced regrowth of fully pigmented hair from the beginning of hair growth, compared to 96% of the PRP patient group8,11.
PRP in androgenic alopecia

The anti-apoptotic effect of PRP has been postulated as one of the important factors in promoting hair growth8,10. The activation of some of the anti-apoptotic regulators (such as Bcl-2 and Akt) has been shown to prolong the dermal papilla and hair cycle9,12. In addition to clinical observation, the results of PRP treatment have been proven histologically, where there was a clear proliferation of the epidermal basal and follicular bulge cells12,13. Additionally, immunohistochemistry showed increased expression of ki67+, a known proliferative marker13. As a result, PRP has shown to improve the mean hair count, mean hair thickness, and mean 2-point score13. The 2-point score is the distance between two hair follicles. The shorter the distance the better, so a shorter 2-point score implies a fuller scalp.
One study looked at the efficacy of adding CD 34+ cell-containing PRP for FPHR and MPHR14. Although the sample size was small (13 patients), patient displayed improvement in mean hair count, mean hair thickness, and mean 2-point score14.
Combination therapy
Although more studies are needed to evaluate the efficacy of combination therapy of PRP with other agents in treating pattern hair loss, the current conducted studies have shown some positive outcomes. One study examined the addition of PRP to follicular unit transplantation15. The study was performed on 20 males with MPHR and the effect of platelet growth factors were significant in patients who received the PRP compared to the ones who did not15,16. PRP has also been used in hair transplantation to reduce swelling and pain18.
Another study combined PRP with herbal extracts17. It was found that the combination therapy resulted in significant proliferation of dermal papillae cells at concentrations ranging between 1.5–4.5%17. The study found that this combination therapy affected the expression of ERK and Akt pathways and thus enhanced the proliferation of dermal papillae cells17. However, more studies are still needed to evaluate the efficacy of combining PRP with herbal extracts.
As to combining PRP with either minoxidil or finasteride is yet to be evaluated since PRP is usually given as a second-line treatment following failure or intolerance to both. Despite the current level of evidence and clinical observation with regards to the beneficial effects of PRP on hair rejuvenation, questions remain regarding the optimal amount, concentration, frequency, and possible synergistic effect through combination therapy in hair rejuvenation. Future studies and trials will hopefully aim to shed light on some of these questions.
Conclusion
In conclusion, regenerative medicine has come a long way and PRP is gaining more interest in the field of dermatology and aesthetic medicine due to its rejuvenating effect on cells. So far, PRP has shown some very promising results in hair rejuvenation through prolongation of the anagen phase and signaling some complex pathways involved in hair growth cycle. The results showed enhanced proliferation, differentiation, and angiogenesis of the derma papillae cells and stem cells in the bulge. Clinically, observed outcomes included increased hair count and enhanced hair thickness. Additionally, these results were achieved with a relatively acceptable cost and a good safety profile. More studies are needed with larger samples sizes and a more detailed evaluation of the long-term effects of PRP. Other modalities have been tried for hair growth and restoration like low-level light lasers and light-emitting diodes18. Their mechanism of action have not been fully understood yet but one theory suggests that they increase adenosine triphosphate, which accounts for hair growth18. Unfortunately, there are not enough studies comparing PRP to low-level light lasers or LED therapy for hair restoration. More comparison and combination studies are needed to enhance our understanding of PRP therapy and its efficacy compared to other treatments.