Study objective
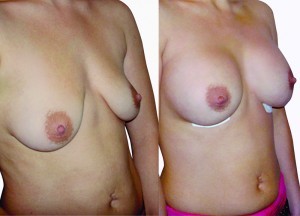
In this study, the authors aim to prove the safety and efficacy of the hydrophilic gel AQUAFILLING® over a long-term post-treatment monitoring of patients after breast plastic surgery.
Study design
A retrospective multi-centre reference-controlled study enrolled 112 subjects, who underwent breast plastic surgery with the application of hydrophilic gel.
Conclusions
Hydrophilic gel is highly safe and efficient. The gel proved its long-lasting efficacy.
The improvement of breast volume and shape, and the removal of asymmetry and deformities of the soft breast tissue is a significant problem for surgeons. At present, breast augmentation with shell silicone implants is the usual method of minimally-invasive breast plastic surgery. Each plastic surgeon faces the risk of unsatisfactory results and undesirable long-term effects or complications after breast plastic surgery performed with silicone implants.
Lipofilling is an alternative procedure of minimally-invasive breast plastic surgery. It provides the patient with a temporary, short-term result, and does not resolve the problem of aesthetics. Ultimately, this method will cause calcinate formation, fibrosis capsular contracture, uneven distribution of the transplanted fat, and the appearance of apparent deformations. In this study, the authors assessed the safety and efficacy of using hydrophilic gel in breast plastic surgery.
Materials and methods
This was a retrospective, multi‑centre, reference-controlled study of 112 subjects, who underwent breast plastic procedures with the application of hydrophilic gel. This clinical study was retrospective and combined outcomes received in a number of specialised institutions performing dermal fillers treatments, including that of the AQUAFILLING gel. As this was a retrospective study, clinical units conducted the enrolment of patients in no particular order. A patient was considered anyone who applied to a clinic and provided a signed patient informed consent form and compliance with inclusion criteria. The data gathering for the statistical analysis was conducted between 2006 and 2012. From 2011, the patients had a supervision period of up to 12 months; 83 patients (74% of all subjects) gave their permission to show their photos in publications and reports.
Subjects and treatment
Subjects eligible for treatment were women aged 18 years and older. A total of 56.3% of subjects were reported as having Fitzpatrick skin type III; 30.4% were type II; 7.1% were type IV; and 6.3% were type I.
Subjects were not considered for enrolment if any of the following exclusion criteria applied:
- Younger than 18 years of age
- Poor mental health Apparent ptosis (type 2–3)
- Mastopathy Within 9-months post-pregnancy
- Very small distance from the teat to the submammary fold
- Problems with blood coagulation, menstruation abnormalities
- Anticoagulant or aspirin intake
- Skin infection or inflammatory disease
- Permanent implants
- Acute contagious diseases of specific and non-specific aetiology
- Chronic contagious diseases in sustained remission stage or recrudescence
- Intolerability or allergy to medicines
- Vessel diseases of different aetiology
- Severe general somatic diseases
- Cancers.
All subjects were divided into four groups depending on treatment goal:
- Breast augmentation in cases of mammary aplasia:14.3% (n=16)
- Breast augmentation: 67% (n=75)
- Correction of asymmetry of breast soft tissues: 6.3% (n=7)
- Correction of ptosis: 12.5% (n=14).
Ninety-two patients (82.1%) were followed-up 3 months after the procedure; 50.9% (n=57) to 6 months; 40.2% (n=45) to 12 months; and 18.8% (n=21) to 3 years.