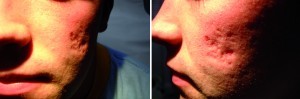
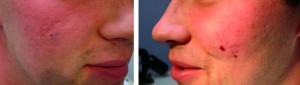
The use of dermal fillers
At the present time, the use of CaHA is approved by the Food and Drug Administration (FDA) for the correction of moderate to severe facial wrinkles and folds19, 20. CaHA also gained prominence during the period in which dermal fillers were being used for antiretroviral-induced facial lipoatrophy21, 22. It is known to cause persistent nodules in a small percentage of people, especially if it is injected into the vermillion border of the lips23. As many studies have established the biocompatibility and safety of CaHA in facial filling techniques21, the product has gained popularity in the US and Europe for this indication, and more recently in the treatment of acne scarring24.
HA has been used in aesthetic medicine for a long time, and has an extended safety profile. In its natural form HA has a short duration time in the tissue, owing to enzymatic degradation and free radical metabolisation. To avoid these effects, HA gel is modified through cross-linking to form a water-insoluble polymer hydrogel, more resistant to degradation, but with a similar biocompatibility as non-modified HA. Based on the experience of other authors, many of the available HA preparations are too short-lived (approximately 3–6 months24, 25 to appropriately treat moderate to severe acne scars) and use of such products for this purpose would require a significant total injection volume over time, with frequent re-treatments, contributing to a greater total cost and time commitment for the patient.
More viscous forms of HA, such as Perlane® (Medicis Aesthetics, Inc., Scottsdale, AZ) or Juvderm® VOLUMA (Allergan, Inc., Santa Barbara, CA), may be appropriate for patients with atrophic scars. The ideal filler for this purpose would be long-lasting, biocompatible, and would not elicit further inflammation or granuloma formation in skin already damaged by acne26.
Soft tissue filler use for acne scarring would be an attractive option to most practitioners as they require little invasive technique and could be used in combination with other treatment modalities, such as microneedling or laser resurfacing. Although studies have shown that HA injections do stimulate collagen formation in the short term, this effect is probably more related to the physical act of injection, rather than to the HA itself.
Subcision is a term introduced by Orentreich and Orentreich27 to describe the minor surgical procedure for treating depressed acne scars and wrinkles, using a hypodermic needle inserted through a puncture in the skin surface and its sharp edges manoeuvred under the defect to make subcuticular cuts or ‘cisions’. The principle of this procedure is to break the fibrotic strands, which tether the scar to the underlying subcutaneous tissue. The depression is lifted by the releasing action of the procedure, as well as from connective tissue that forms during the course of normal wound healing28.
Methods
A series of 27 patients (17 male, 10 female; skin phototypes I–IV), with varying degrees of atrophic acne scarring, were treated in a single-centre, prospective, controlled study over a 1-year period.
Patients were randomly selected on the basis that they did not want to present for laser resurfacing as a treatment for their problem. This meant the patients were enrolled sporadically, rather than entering the study at the same time. The subjects ranged in age from 16–63 years, and all acne scarring severity scores fell between 4 and 30 on the Goodman system. Patients were also evaluated using digital photography and an improvement graduation scale at each subsequent treatment visit, at 1, 3, 6, 12 and 24 months post-procedurally:
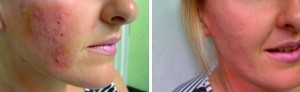
Figure 2 23-year-old female patient (left) during treatment with Radiesse, and (right) 2 weeks after treatment
-
0 = no improvement
-
1 = 0–25% improvement
-
2 = 25–50% improvement
-
3 = 50–75% improvement
-
4 = 75–100% improvement
-
5 = 100% improvement.
Multiple acne scar grading classification systems of varying complexities have been introduced. The most basic, practical system divides atrophic acne scars into three main types: icepick, rolling, and boxcar scars29. It is common for patients to have more than one type of scar.