Combination superficial peels
Combination peels aim to achieve a synergistic interaction of their components, with regard to either efficacy or safety. Despite the scarcity of evidence to support their superiority, combination peels are considered to be a current trend in chemical peeling.
Medium depth peels
The main clinical indications for medium depth peels include dyschromia (mainly solar lentigines), multiple solar keratosis, and textural changes of the skin. Wrinkles and acne scars can be improved only slightly, and deeper treatment modalities are usually required to provide a more significant improvement in these cases.
Trichloroacetic peels
TCA can be used in different concentrations. A 10–20% TCA peel is used for superficial peels, while 35% is used as a medium depth peel. Concentrations higher than 35% are not recommended as the results are less predictable and the potential for scarring is higher. In order to increase the depth and efficacy of the TCA peel, without increasing the concentration of the acid, it has been suggested to combine this chemical with Jessner’s solution (Monheit method)9, 70% glycolic acid (Coleman method), or solid CO2 (Brody method).
The TCA solution is compounded in a weight to volume preparation. To prepare a 35% solution, 35 g of TCA crystals are dissolved in a small amount of water, then further water is added to make a total volume of 100 mL. TCA is stable at room temperature and not light‑sensitive.
TCA peeling is a painful procedure; therefore, local injection anaesthesia or intravenous sedation should be considered. A patient usually becomes completely comfortable 15–20 minutes after the procedure, when the frosting subsides.
During the procedure, TCA is painted using a q-tip according to the cosmetic units and until a white frost appears. The degree of the frosting correlates with the depth of solution penetration:
- Level I is speckled white frosting with mild erythema and corresponds to superficial penetration
- Level II is characterised by an even white-coated frost with background erythema. This degree of frosting is usually desirable for medium depth peels
- Level III is solid white opaque frost with little or no background erythema, usually characterising deep peels and not desirable in a TCA procedure.
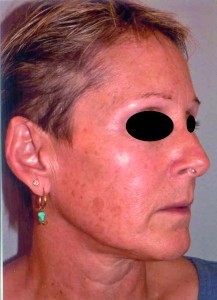
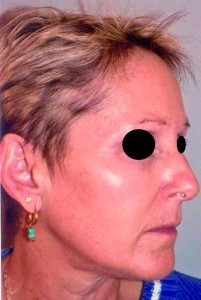
During the first few days after the peel, patients are expected to feel a tightening and swelling of the skin, as post-peel, the skin starts to crack and desquamation begins. Full re-epithelisation is usually complete after 5–7 days (Figure 2).
A 35% TCA peel can be combined with Jessner’s solution (resorcinol 14%, lactic acid 14%, and salicylic acid 14% in alcohol), solid CO2 10, or 70% glycolic acid11.
Deep peels
The main indications for deep chemical peels include dyschromia, fine and coarse wrinkles, pre-malignant skin tumours, and acne scars. Deep peeling solutions penetrate to the mid-reticular dermis and create the maximum effect for the production of new collagen. The solutions for deep peels are composed of a combination of croton oil and phenol at different concentrations. Phenol is an aromatic hydrocarbon originally derived from coal tar. Croton oil is an extract of the seed of the plant Croton tiglium, which causes skin vesiculation. Other chemicals in use in deep chemical peel formulae include septisol, water, and vegetable oils (glycerin, olive, sesame)12.
A phenol-based peel is carried out under full cardiopulmonary monitoring with intravenous hydration throughout the procedure. Intravenous sedation or regional blocks make the procedure pain‑free. For application of the peeling solution, cotton‑tipped applicators are used. The usual end-point is an ivory–white to gray–white colour of the skin. Immediately after the face is covered with the solution, waterproof zinc oxide non-permeable tape is applied to the skin. After 24 hours, the tape mask is removed and the skin exudate is cleaned using sterile saline. The face is covered with bismuth subgalate antiseptic powder for 7 days. Other options include occlusive moisturisers, antibiotic ointments, and biosynthetic occlusive dressings. After the skin has achieved a full re‑epithelisation, the powder mask is removed (usually at 8 days post-peel) and the patient is advised to use water‑based lotion creams and potent broad-spectrum sunscreens. The erythema gradually subsides over a period of approximately 2 months. During this time, make-up with a green foundation is encouraged to allow the patient to resume all daily activities. In cases of olive‑skinned patients, the application of Kligman preparation is recommended to prevent reactive hyperpigmentation.
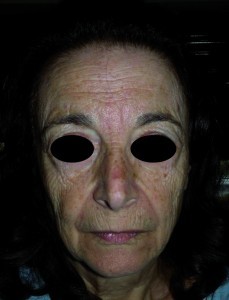
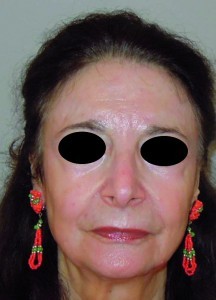
Deep peels are considered to be the most powerful non-surgical method for facial skin rejuvenation, and the term a ‘non-surgical face lift’ has been coined to describe this procedure (Figure 3).