To determine the best plan for every patient, there are many variables to be considered, including the patient’s age, body type, surgical history, tumour size, stage of cancer, previous treatment with radiation, and insurance coverage, along with the patient’s preferences. It is important to remember that there is a lot at stake for the patient. She will have to live with the consequences of this potentially life-altering decision, and therefore, she should ideally play an active role in the decision-making process.
There are concerns regarding breast cancer patients’ access to breast reconstruction, which has been shown to provide important psychosocial benefits. Breast reconstruction has increased over time, but it has wide geographic variability. Many women who face a cancer diagnosis are not informed of the reconstruction options available to them. Further research and interventions are needed to ensure equitable access to the multidisciplinary treatment of breast cancer1.
New trends in breast reconstruction
According to the American Society of Plastic Surgeons (ASPS), 95589 women underwent breast reconstruction in 2013 in the US, a 21% increase since 2000. A total of 76078 women opted for implant reconstruction. Of these, 19511 women underwent flap reconstruction, the majority of which were deep inferior epigastric perforators (DIEP), latissimus dorsi, and transverse rectus abdominis myocutaneous (TRAM) in descending order2.
One of the most notable trends is that nipple-sparing procedures are becoming an increasingly common choice for women undergoing mastectomy. Although considered a relatively new and technically challenging procedure, more surgeons are now offering nipple sparing mastectomy (NSM) to patients who are candidates.
According to plastic surgeon Aldona J. Spiegel, at the Institute for Reconstructive Surgery at Houston Methodist Hospital, in Houston, TX, ‘Among the new trends in reconstructive breast surgery is composite reconstruction that combines several procedural modalities to improve outcomes. These procedures include fat grafting to fill in thin areas or irregularities in the mastectomy, combined with the use of collagen over the implant for optimal aesthetic results. Also, over the last 5 years, nipple sparing mastectomy has become a more popular choice in select patients because it results in a more natural appearance where the scar is hidden under the breast.’
However, as Spiegel cautions, not every patient is a candidate for this option. ‘A lot of the modalities we can choose from will depend on the patient,’ she said. ‘Another trend in this field is where patients choose to use their own tissue, for example a DIEP flap combined with an implant. The implant is used like an augmentation to add conical projection, since abdominal tissue is maybe too flat to give adequate projection. This may greatly improve the final result in select cases. By combining a nipple sparing mastectomy with a DIEP flap and an implant, you can achieve a ‘mommy makeover’ result in patients who are candidates for that procedure.’
She adds, ‘For women who are not candidates for flaps, we can offer them composite breast reconstruction by using ADM (collagen) as a hammock for the bottom part of the implant, where the top is covered by pectoral muscle. We can also do fat grafting (liposculpting) over the muscle and ADM to camouflage the implant. In cases with radiated skin, this improves the quality of the skin. In nipple sparing mastectomies, the tissue under the nipple is removed, which flattens the nipple. We can then improve the projection of the nipple by performing fat grafting.’
According to Birmingham, AL plastic surgeon James C. Grotting, President-Elect of the American Society for Aesthetic Plastic Surgery (ASAPS), ‘Among the trends in breast reconstruction over the past several years, we have seen that autologous reconstruction fell quite a bit, from over half of women getting flaps, to now about a quarter of women. This can be attributed to the fact that women in general prefer to have less surgery. They are reading about quick recovery and that is what they want,’ he said. Another reason he cites is that implants have greatly improved. ‘Saline implants have been replaced with silicone gel that are far superior. High cohesive anatomical gel implants are most appropriate in reconstruction, at least in the US market. In many cases, women cannot afford to do autologous flap procedures, which involve a much longer recovery and hospitalisation that is not always covered by their insurance. You can get reasonable results with implant reconstruction alone.’
‘Another trend we are seeing is that bilateral procedures are becoming more common as preventative measures. Conservation treatment is not as popular now, as long term results have been evaluated and oncologists are seeing that there is a strong case for bilateral mastectomy, especially among women who are BRCA positive,’ he said.
Grotting adds that flaps in reconstruction are more frequently used as perforator flaps, where the surgeon tries to take little or no muscle with the flap. ‘This has resulted in an explosion of new donor sites. The abdomen is far and away the best donor flap for breast reconstruction because it happens to be an area of most women’s bodies where fat exists in excess, and skin is loose enough so in the right candidate you can end up with enough tissue to create a natural appearing breast. You can do it as a pedicle tram, muscle sparing free tram or DIEP flap. The important thing is that you leave the abdomen functionally reconstructed and leave only healthy tissue with good blood supply. Good results can be achieved with any of these techniques.’
Novel products for optimal results
Until recently, surgeons had the choice of porcine, bovine or human acellular dermal matrices for use in immediate breast reconstruction. New methods of harvesting and processing autologous fat, variations on surgical mesh, fat used in combination with ADM, and other techniques are revolutionising the way plastic surgeons are perfecting their results even in challenging cases like secondary reconstruction.
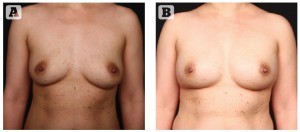
Figure 1 (A) Preoperative view of 35 year old female with BRCA positive gene. (B) A 1 year postopeartive view of the patient following two stage reconstruction with expander, Alloderm (LifeCell Corporation, Bridgewater, NJ), and injection of Botox (Allergan, Irvine, CA) at first stage followed by placement of Natrelle 410 MF implants (Allergan, Irvine, CA) and fat injection. © Courtesy of Allen Gabriel, MD
The SERI® Surgical Scaffold technology from Allergan (Irvine, CA) shows promise as an off-the-shelf, long-term bioresorbable scaffold for support and repair of weakened or damaged connective tissue. As patients are sometimes concerned about human-derived tissue implants, one of the main advantages of the new SERI® Scaffold is that it is composed of a bioresorbable surgical scaffold made out of a proprietary silk-based material. In Europe, at the current time, the product is not commercially available.
Fat grafting as an aesthetic refinement procedure in breast reconstruction has become a mainstay all over the world. ‘Autologous fat grafting is the future of breast reconstruction. Short of being able to grow a breast in vitro, and that is where we might be some day as fat grafting techniques keep improving. You can combine fat grafting with implants to produce a very natural and beautiful breast,’ said Grotting. ‘I prefer to use the patient’s own natural tissue to support an expander or an implant in place.’
Spiegel is an enthusiastic proponent of the PureGraft (Puregraft LLC, San diego, CA) system. ‘I really love PureGraft. I am now adding fat grafting to most of my breast reconstruction procedures. I usually liposculpt around the flap or implant and I use fat as an adjunct in reconstruction. You have to be very careful that you are not doing anything to the donor site that would cause contour irregularities, which is more difficult in thinner patients.’
The combination of several key components that compliment each other in various ways can produce beautiful results for patients. The concept of the ‘bioengineered breast’ was originally developed by plastic surgeons G. Patrick Maxwell and Allen Gabriel in 2007 when they were using acellular dermal matrix, fat grafting, and highly cohesive gel fifth generation implants. ‘Cells, scaffolds and fifth generation implants are utilised to create the bioengineered breast which creates a more natural shape,’ said Maxwell.
‘This concept has set a new standard in breast cancer reconstruction, allowing women less invasive mastectomies with reconstruction, which often leaves a better cosmetic outcome than the patient’s natural breasts. Not only is the appearance of the reconstructive breasts superior, but the feel of the breasts remain soft and natural over time.’ said Gabriel.
‘A quality of life study in these patients has documented that superior cosmetic results in breast cancer reconstruction lead to an improved quality of life,’ said Maxwell. ‘This same concept of ‘bioengineered breasts’ can be applied to risk reduction mastectomies for ‘prevention’ of breast cancer as well as primary and secondary cosmetic surgical procedures of the breast,’ he added. The authors have the world’s largest experience and clinical series.
According to Dr Marissa Tenenbaum, Assistant Professor of Surgery, Division of Plastic and Reconstructive Surgery, Washington University School of Medicine in St. Louis, MO, ‘I use the HydraSolve system from Andrew Technologies (Tustin, CA) for fat grafting in breast reconstruction. The quality of the fat and the ease of use are exceptional. I am seeing a lot less fat necrosis after moving to this technology.’
Patient-centred techniques are changing the landscape
In this day and age, insurers, institutions, and providers are more focused than ever on reducing recovery time for patients, and minimising complications and the need to bring the patient back for additional surgery. Plastic surgeons are also intent on improving outcomes for their patients.
Laser-assisted indocyanine green angiography is a relatively new tool for determining whether mastectomy skin flaps have adequate blood supply. The SPY Elite® System (LifeCell Corporation, Bridgewater, NJ) enables surgeons to assess tissue viability with real-time information that may be used to modify operative plans and optimise outcomes before the patient leaves the operating table.
According to Grotting, ‘The SPY scanner is helpful in surgery to tell you whether the mastectomy skin flaps are good. When the procedure is complete, surgeons can use the scanner to see if the flaps are good, and if adjustments are needed, they can reoperate right then. It can potentially reduce the complication and revision rate for immediate breast reconstruction. You can be surprised that tissue that looks healthy, when you scan it, is not.’
According to Speigel, ‘Restoration of nipple sensation is now also possible using a new method of DIEP flap nerve regeneration using the third anterior intercostal nerve. By connecting the nerve from a flap to the mastectomy nerve we can restore sensation, which is an area that is frequently not discussed and is usually not a procedure covered by insurance. This technique provides a significant increase in sensory recovery for breast reconstruction patients, while adding minimal surgical time. It is difficult because you have to find a sensory nerve and anatomically, this is not so easy to locate.’ 3
Botulinum toxin (BOTOX® Allergan, Irvine, CA) was shown to effectively address the source of severe pain associated with expanded/implant based breast reconstruction following mastectomy. According to Vancouver, WA plastic surgeon Allen Gabriel, ‘We no longer do a single breast reconstruction case without using BOTOX. Implant based breast reconstruction involves implantation of a temporary expander under the pectoralis major chest muscle, which is filled with saline serially to create a pocket where a permanent implant will reside. The muscle often contracts and spasms in response to the expansion, causing pain,’ he said.
In collaboration with Nashville, TN plastic surgeon and inventor, G. Patrick Maxwell, MD, they theorised that injections of botulinum could offer relief by temporarily paralysing the muscle, causing it to remain flaccid so that fewer spasms would occur and less pain would arise.
In their study, the women who received the botulinum injections were far more comfortable after surgery than those who received placebo. Drs Gabriel and Maxwell found a statistically significant increase in the volume of expansion per office visit, leading to full expansion more quickly in the botulinum group than in the placebo group. ‘Our average expansion time is less due to improved pain management with BOTOX®. We take a 100 unit bottle, add 5 ccs saline, and we inject 2.5 ccs on each side during the time of the primary reconstruction,’ said Gabriel. ‘Patients are happier, and the they are more comfortable during this phase.’
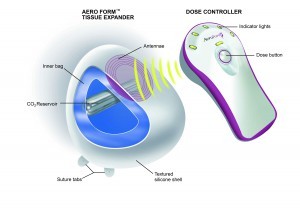
The AeroForm™ Tissue Expander (AirXpanders Inc, Palo Alto, CA) is an investigational device in the US that is poised to have a significant impact on reconstructive surgery. This novel patient controlled breast tissue expander that includes a small handheld wireless controller that administers small amounts of CO2 into the device to stretch the skin to accommodate a permanent breast implant. AeroForm allows women to complete their expansion at home, without needles and at their own pace based on their level of comfort. According to Dr Kamakshi Zeidler a plastic surgeon in San Jose, CA, and principal investigator of the clinical trial, ‘Breast reconstruction post mastectomy is a long process, and tissue expansion is one of the most tedious and painful aspects. For women to achieve expansion in 19 days on average and for the vast majority of patients to report high satisfaction throughout the expansion process, supports AeroForm as an exciting, much-needed innovation in breast reconstruction,’ she said. ‘Allowing women to expand at their own pace and level of comfort, offers mastectomy patients a convenient and needle-free option for expansion — and a chance to regain control over their body at a time when it is out of their control.
More choices offer optimised results
There are three manufacturers in the US currently offering shaped silicone gel implants cleared for marketing by the FDA; Sientra (March 2012), Allergan (February 2013), and Mentor (June 2013)4.
‘The more choices we have, the better we can tailor the operation to each patient,’ said Spiegel, noting the recent FDA approval of additional MENTOR MemoryShape® (Mentor Worldwide LLC, Santa Barbara, CA) implant styles. MENTOR® MemoryShape® Breast Implants have a teardrop shape, much like the silhouette of a natural breast and are filled with a cohesive gel that enables shape retention. ‘We needed these higher projecting implants, which are important to get the best results,’ she said.
The future of breast cancer therapy
A Hungarian born material scientist at the University of Akron, OH, Judit E. Puskas, PhD, P.Eng, is pioneering a unique polymer that is not permeable, unlike silicone, and can also be used as a way to deliver drugs for cancer, such as tamoxifen or chemotherapy drugs. ‘New delivery devices are badly needed for cancer therapy. Specific targeting is the optimal approach for any diagnostic and chemotherapeutic agent. The goal of our research is to integrate breast reconstruction with cancer diagnosis and treatment. The implant becomes a medical device itself. If the drug is delivered intravenously, a higher concentration must be used. By using a lower concentration, you can have less side effects for the patient,’ said Puskas. ‘First I would like to use my polymer as a cover or coating for existing implants, then we would like to replace the silicone shell, and then we can work on developing an all polymer gel as a filler for breast implants.’
Detecting breast cancer at an early stage is crucial to save lives. University of Nebraska-Lincoln scientists have developed a nanoparticle-based device that emulates human touch and that could significantly enhance clinical breast exams for early detection of cancer5. Researchers Ravi Saraf and Chieu Van Nguyen developed a thin-film sensor, like an ‘electronic skin’, that can detect tumours too small and deep to be felt by human touch. The thin film is only one-sixtieth of the thickness of a human hair and is made of nanoparticles and polymers, which when pressed against the skin, creates changes in electrical current and light that can be captured by a high-quality digital camera. Using a silicone breast model, the researchers used the film to successfully detect tumours as small as 5 mm, hidden up to 20 mm deep. The technology would also allow improved detection for skin cancer.
Lastly, adds Grotting, ‘It is rather short sighted for plastic surgeons to think that these implants are going to last forever for patients. One of my least favourite operations is to take broken silicone gel implants out. In most cases, clinical findings are minimal to none with ruptured implants. You have to rely on whether the patient has seen a change, which would then prompt an MRI. I am recommending that we have a conversation with every gel patient at 10 years to consider preventatively changing the implants for a fresh device. It is still very difficult to make the diagnosis of a broken implant, and implant failures may be missed. I think of it as analogous to changing the tyres on the car before you have a blowout on the interstate,’ he said.