Tissue remodelling
Autologous PRP has attracted attention in a number of medical fields. In one study34, the effects of activated PRP (aPRP) and activated platelet-poor plasma (aPPP) were investigated with regard to the remodelling of the extracellular matrix (ECM), a process that requires activation of the dermal fibroblasts—essential for the rejuvenation of aged skin. aPRP AND aPPP both stimulated cell proliferation, with peak proliferation occurring in cells grown in 5% aPRP. Additionally, aPRP and aPPP increased the expression of type I collagen, MMP-1 protein, and mRNA in human dermal fibroblasts.
aPRP and aPPP promote tissue remodelling in aged skin and may be used as adjuvant treatment to lasers for skin rejuvenation in cosmetic dermatology. Although the optimal platelet concentration is unclear, the current methods by which PRP is prepared is reported to involve approximately 300–700% enrichment, with platelet concentrations consequently increasing to greater than 1000000 platelets35. These factors are known to regulate processes including cell migration, attachment, proliferation and differentiation, and promote ECM accumulation by binding to specific cell surface receptors36.
In the dermis, which is continually exposed to UVB, collagen degeneration and altered deposition of elastic tissue result in the impairment of the structural integrity of the dermal ECM, causing the skin to wrinkle. The skin’s resilience is also reduced. Compared with the serum-treated control group in one study37, aPRP and aPPP showed a marked increase in fibroblast proliferation. Cells exposed to 5% or 10% aPRP also exhibited significantly higher rates of proliferation than positive control cells. These results indicate that aPRP and aPPP promote the proliferation of fibroblasts. On the other hand, the expression of the a1 and a2 chains of type I collagen was increased in cells treated with 5% aPRP or aPPP (compared with negative control), suggesting that both PRP and PPP show an ability to induce collagen production.
This stimulation of de novo collagen synthesis may compensate for the defects that arise as a result of the fragmentation or loss of collagen in photoaged and aged skin. Accumulation of this newly-synthesised collagen may improve the structural integrity of the dermal ECM and stimulate fibroblasts to produce more collagen. Similarly, induction of MMP-1 in photoaged skin may facilitate the removal of collagen fragments that damage the dermal matrix tissue, thus providing a better foundation for the deposition of new collagen38. In a more recent study, injection of PRP in the face and neck for revitalisation obtained good results39.
PRP treatment results
PRP combined with fractional laser was found to increase patient satisfaction and skin elasticity, and decrease the erythema index40. Furthermore, treatment increased the length of the dermo–epidermal junction, the amount of collagen, and the number of fibroblasts. PRP with fractional laser treatment is a good combination therapy for skin rejuvenation. Keratinocyte and fibroblast proliferation and collagen production can explain the capacity of PRP to increase dermal elasticity.
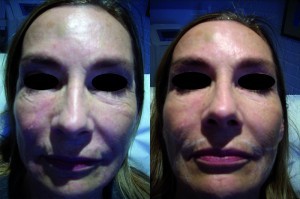
In a study to evaluate the efficacy of a single injection of autologous platelet-rich fibrin matrix (PRFM) for the correction of deep nasolabial folds (NLFs), whole blood was obtained from 15 adults, and an activated autologous platelet-rich fibrin matrix produced using a proprietary system1. It was then injected into the dermis and immediate subdermis below the nasolabial folds. Subjects were photographed before and after treatment; folds were rated by the treating physician before and after treatment using the Wrinkle Assessment Scale (WAS), and patients rated their appearance at each post-treatment visit using the Global Aesthetic Improvement Scale (GAIS). Patients were evaluated at 1, 2, 6, and 12 weeks post-treatment.
All patients were treated to maximal (no over-) correction, with a mean reduction in WAS score of 2.12 +/- 0.56. No patient noted any fibrosis, irregularity, hardness, restricted movement, or lumpiness. The author of the study concluded that PRFM can provide significant long-term diminution of deep nasolabial folds without the use of foreign materials. PRFM holds significant potential for stimulated dermal augmentation. (NB. The system used in this study uses thrombine to get a stronger fibrin mesh and therefore cannot be defined as 100% autologous.)