Dr. Giuseppe Scarcella discusses his experience using picosecond lasers to treat pigmented lesions

The treatment of pigmented lesions aims to remove the undesired excess of pigment, saving the constitutional pigment and the surrounding structures. Melanin is a good target for laser light because of its wide absorption spectrum (from 250 to 1200 nm). Theoretically, every laser producing ultraviolet, visible or infrared radiation, can remove the undesired pigment more or less effectively.
It is far easier to remove epidermal pigment, which is more superficial than treat dermal pigment that requires more sophisticated systems to be treated with to avoid side-effects1,2.
The absorption of laser light by the skin chromophores depends on the chosen wavelength (λ). A selective window for melanin is between 500 and 1100 nm; this represents a range of λ with better skin penetration and better selectivity of absorption by melanin rather than other chromophores, most of all, oxyhaemoglobin. Another important aspect is to confine thermal damage to produce selective photo-thermolysis. By using pulsed lasers with appropriate pulse duration, it is possible to minimize the diffusion of heat and consequently, the thermal insult towards the structures adjacent to the target itself. Exposure times lower than the Thermal Relaxation Time (TRT) of the pigmented target will selectively destroy it, sparing the surrounding structures. Hence, pulsed lasers with appropriate λ have a clear theoretical advantage over continuous lasers in destroying skin pigment selectively3, 4.
In treating pigmented lesions, the main target of the laser is the melanosome: with a diameter of about 1μm, it has a Thermal Relaxation Time of no more than 1μsec. Therefore, any laser pulse of a microsecond or less can destroy it in a selective way.
The mechanism managed by pulsed lasers to destroy the melanosome is not yet fully understood. It is believed that the damage to the melanosome is caused by its rapid and selective heating and by the shock wave or cavitation damage resulting from the rapid thermal expansion, due to the extreme temperature gradients created between the inside and outside of the melanosome. Studies on the acoustic waves generated by the pulsed irradiation of melanosomes and pigmented cells support this theory; thus, this reaction is called the ‘photoacoustic effect’. Melanin absorbs and localizes the high radiation intensity of the Q-switched lasers typically used in the treatment of these lesions (i.e. lasers capable of generating enormous fluences in a very short time) in order to create a clear temperature gradient between the melanosome and its surroundings. This gradient involves thermal expansion and leads to the generation and propagation of acoustic waves that can mechanically damage cells loaded with melanosomes5.
Histologically, the destruction of melanosomes and the damage to the cells that contain melanosomes occurs immediately after laser irradiation. The cells (keratinocytes and melanocytes) undergo a phenomenon of vacuolization; this phenomenon results in epidermal necrosis, followed by subsequent and complete recovery in about seven days.
The exposure threshold that creates the aforementioned damage in the melanosome is represented by a typical immediate skin whitening, that can be observed clinically when pigmented lesions are treated with this kind of laser radiation.
Similar melanosome alterations have been observed at different λ; however, they differ in terms of dose-threshold and dermal penetration. In general, less energy is needed using shorter λ, while more energy is required with longer ones due to the decrease in melanin absorption selectivity when λ increases. Therefore, longer λ have the ability to attack the deep pigment, while shorter ones can attack superficial pigmented lesions even with lower energies.
Dark photo-type patients can be treated with greater difficulty, especially in the case of dermal lesions, since their high epidermal melanin concentration can compete with the underlying melanin that is the target of the treatment. These patients should be treated with caution, using usually lower fluences and should be informed about the possibility of hypo-and hyperchromic side-effects that are almost always solvable, and about the almost certain need of some additional sessions.
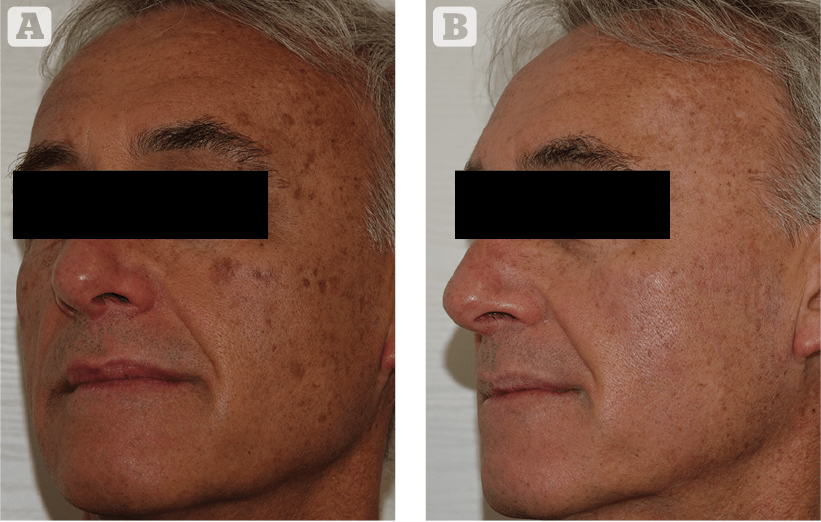
A variety of laser systems are available for the treatment of pigmented lesions. The choice of the right laser must be based on the type of pigmented lesion (superficial or deep), on the patient’s phototype, and on the reaction of each kind of lesion to the various lasers.
The Q-switched nano- and picosecond lasers are the most suitable and the best performing methods for the treatment of pigmented skin lesions. In this article, we will examine the results that can be obtained in this field with the use of Candela’s PicoWay, a 4-wavelength picosecond laser system.
The high peak power of PicoWay involves greater efficacy and safety. The 450ps pulse at 1064 nm and the 375ps at 532 nm of the PicoWay delivers 4.5 times more photoacoustic effect than the lower energy pulse of other picosecond lasers. The longer pulse-width of the other laser generates mostly thermal energy delivered over a longer period of time. The thermal energy is the main source of side-effects and lower efficacy, so the PicoWay can provide higher efficacy and less discomfort. Laser energy is delivered so rapidly that even the smallest pigment fragments will shatter, and this is necessary for the elimination of different kinds of tattoos, as well as pigmented lesions.
The main features of PicoWay are:
- Four highly effective wavelengths (1064 nm, 730nm, 532 nm and 785 nm at 300 ps) in one picosecond system
- 40%–50% shorter pulses, which mean highly effective treatments with lower fluences for results with low risk of side-effects
- Highest peak power for effective treatment energy over the broadest range of spot sizes
- Four wavelengths to treat most tattoo colours and types, including recalcitrant tattoos and different kind of pigmented skin lesions (epidermal, dermal and mixed), and
- Large spot sizes, with effective fluences, that enable deep penetration when needed.
Finally, with the use of the holographic picosecond fractional handpiece — RESOLVE, we are able to eliminate cutaneous pigmented lesions with very little discomfort for patients (almost no downtime). Fractional technology induces an optical breakdown in the dermis while leaving the epidermis intact. These lesions in the dermis, because of plasma formation, stimulate a healing response and skin remodelling, which results in the elimination of unwanted pigmented lesions and skin rejuvenation. The goal, therefore, is to create an ordered matrix of dermal vacuoles produced by the photomechanical interaction of the Q-switched pulse, commercially called Subsurface Laser Induced Optical Breakdown (LIOBs), without coagulation action and preserving the epidermal layer as much as possible, with the purpose of inducing the tissue to regenerate6–8.
Patients and methods
For treatment with the PicoWay laser, we enrolled patients of different phototypes and with different types of pigmented lesions. The phototypes enrolled were skin type I to V and the pigmented skin lesions treated were solar lentigo, flat and pigmented seborrheic keratoses, Post Inflammatory Hyperpigmentation (PIH), hyperchromic scars, Cafè au Lait spots and melasma. The latter has been treated in different phototypes and in different patterns: epidermal, dermal, and mixed. All these pathologies were treated both with the Zoom handpiece and with the fractionated Resolve handpiece. Except in the case of melasma, the endpoint of the treatment was usually reached after one or a maximum three shots on the same lesion, and consisted of, when using the 532 nm Zoom handpiece, in the appearance of a delicate ‘popcorn effect’ without any appearance of bleeding. Also, when using the Resolve 532 nm handpiece, the site was checked with dermoscopy and the appearance of microscopic areas of crisp whitening ‘micro popcorn effect’ equally free of any bleeding were reported. Finally, in the case of melasma, both with the use of the 1064 nm Zoom handpiece and the Resolve 1064 nm handpiece, the endpoint consisted of diffuse erythema with slight oedema that disappeared in about a day. This endpoint was achieved with the use of very low fluences and with a ‘brushing technique’ consisting of different and repeated laser passes performed in the same session on the same area9–13.
Results
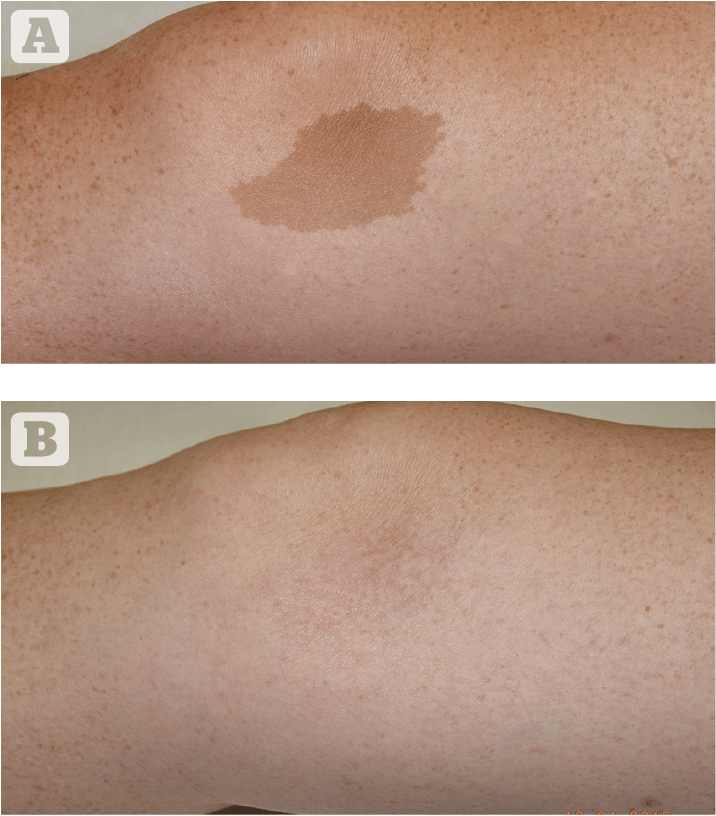
Most solar lentigos, flat and pigmented seborrheic keratosis (incipient seborrheic keratosis) were treated successfully with the 532 nm Zoom handpiece after only one session using the appropriate fluences and spot diameters, and with two or maximum three sessions using the Resolve handpiece 532 nm14,15. The Cafè au Lait spots were treated with an average of three laser sessions using the 532 nm or 785 nm Zoom handpiece and choosing the most effective wavelength after a test performed with both.
Melasma and PIH patients responded well in 80% and 60% of cases, respectively, and with an average of four laser sessions, both with the 1064 nm Zoom and the Resolve handpiece used with the same wavelength. The hyperchromic scars were treated with the 532 nm or 785 nm Zoom handpiece, depending on which wavelength gave the best response in the initial test and resolved in 70% of cases in an average of two sessions. Patients tolerated the treatments very well, and there were no major side-effects or adverse events reported, especially if the Resolve handpiece was used and with both wavelengths supplied.
Discussion
The picosecond laser, PicoWay by Candela, is currently one of the most versatile and effective tools in the world for the treatment of all types of pigmented skin lesions and a range of different phototypes because it has four wavelengths (532, 730, 785 and 1064 nm), one of the shortest pulse widths on the market, very high fluences, and the further addition of the fractional handpiece, Resolve. Furthermore, with its four available wavelengths — that can reach different depths — we can choose the one that best suits the case we are dealing with, and consequently choose the most effective one.

Lesions can be treated with a single laser session in most cases, or with a few sessions depending on the lesion. If the patient wants to eliminate unwanted pigmented skin lesions, reduce discomfort and downtime to a minimum, the Resolve handpiece is the appropriate tool even if we achieve these results perhaps with one or two sessions more than had we used the Zoom handpiece. The best strategy will be choosing the appropriate treatment management according to the individual needs of the patients. Again, with the Resolve handpiece, playing with the various fluences delivered and therefore the different depth of the LIOBs obtained, it is possible to improve significantly the performance of the results achieved in the treatment of the different patterns of melasma: epidermal (superficial), dermal (deep) or mixed.
Finally, we concluded that in dark phototypes PicoWay laser could give excellent results, even if we might have to slightly increase the number of laser sessions. In these cases, both for treatment of melasma or pigmented skin lesions with either the Zoom handpiece or fractionated Resolve handpiece, it is always good practice to reduce the fluences by 20–30% compared to what is used with Caucasian phototypes. Furthermore, in dark phototypes, it is also always a good approach to make a laser-test session before enrolling patients in a complete treatment series.
Conclusion
When we use PicoWay to treat pigmented skin lesions we work with lower fluences; therefore, we cause less pain, discomfort and reduce healing time. We are able to achieve good results with a higher percentage of pigment clearing and can treat dark phototypes better because of the shorter pulse width.
Finally, we cause less discomfort (almost no downtime) with the use of the holographic fractional handpiece, Resolve.
Declaration of interest Funding for submission of this paper was provided by Candela
Figures 1–6 © Dr Scarcella
References
- Sherwood K, Murray S, Kurban A, Tan O. Effect of wavelength of cutaneous pigment using pulsed irradiation. J Invest. Dermatol 1989; 92: 717-20
- Taylor CRFT, Michaud N, Jimbow K, Anderson RR: Q-switched ruby laser of benign pigmented lesions: dermal vs. epidermal. Laser Surg Med 1991, suppl. 3:65
- Goldberg D. Benign pigmented lesions of the skin: treatment with the Q-switched ruby laser. J Dermatol Surg. Oncol 1993; 19: 376-379
- Rosenbach A, Williams CM, Alster TS: Comparision of the Q-switched alexandrite (755 nm) and Q-switched Nd:YAG ( 1064 nm ) lasers in the treatment of benign melanocytic nevi. Dermatol Surg. 1997; 23:239-45
- Scarcella G: Papel del Medlite IV en la fotodepilacion y las manchas cutàneas. Abstracts XIV Congreso Nacional Sociedad Espanola de Medicina estetica. Barcelona, June, 5-7 giugno, 1998
- Habbema L, Verhagen R, Van Hal R, Liu Y, Vargese B: Minimally invasive non-thermal laser technology using laser-induced optical breakdown for skin rejuvenation. J Biophotonics 2012; 5 (2):194-199
- Habbema L, Verhagen R, Van Hal R, Liu Y, Vargese B: Efficacy of minimally invasive nonthermal laser-induced optical breakdown technology for skin rejuvenation. Lasers Med Sci 2013; 28:935-940
- Bernstein EF, Schomacker KT, Basilavecchio LD, Plugis JM, Bhawalkar JD: Treatment of acne scarring with a novel fractionated, dual-wavelenght, picosecond-domain laser incorporating a novel holographic beam-splitter. Lasers in Surg and Med; 2017; 49: 796-802
- Polnikorn N. treatment of refractory dermal melasma with Medlite C6 Q-switched Nd:YAG Laser. Report of two cases. J Cos Laser ther; 2008; 10:167-173
- Polnikorn N.Treatment of refractory melasma with the Medlite C6, Q-switched Nd:YAG lasetr and alpha arbutin. A prospective study. J CosLaser Ther 2010; 12:126-131
- Bevec T et All: Treating Melasma with sub-thermolytic Q-Switched Nd:YAG. Journal of the Laser and health Academy. 2011; n.1
- Mun Young Ji et All: A low fluence Q-Switched Nd:YAG Laser modifies 3d structure of melanocyte and ultrastructure of melanosome by subcellular-selective photothermolysis. Journal of Electron Microscopy; 2011; 60 (1): 11-18
- Scarcella G: Clinical evaluation of the efficacy of a topical lightening product associated with the Q-switched Nd: YAG laser in the treatment of deep face melasma. Journal of Plastic Dermatology; 2013; 9,3
- Scarcella G; Dethlefsen M W, Nielsen Engelbrecht MC: Treatment of solar lentigines using a combination of picosecond laser and biophotonic treatment. International Journal of Dermatology. July, 6, 2018
- Scarcella G, Gerber P, Edge D, Nielsen Engelbrecht MC: Effective removal of solar lentigines by combination of pre-And-post-fluorescent light energy treatment with picosecond laser treatment. Wiley OnLine Library; Clinical Case Report; July, 11, 2020





