Rhinoplasty surgery remains one of the most difficult operations to perform on the face. Improving aesthetic appearance and maintaining nasal function are inseparable goals in rhinoplasty surgery, and failure with either can be devastating for the patient. Owing to the variety of potential rhinoplasty complications, more care and attention should be paid to the surgical technique for reconstruction of the dorsum aesthetic lines and nasal tip projection in patients with a prominent hump. Based on modern cartilage-conserving concepts, the autospreader flap rotation technique should be considered when dorsal reduction is required. Familiarity with aesthetic anatomy and function is fundamental to identify the appropriate indications for this technique, which is a useful tool to prevent postoperative nasal obstruction, segmental appearance, mid-facial axial asymmetry, severe supra-tip break, and to preserve the patient’s ethnicity. Patients with short nasal bones and low lower lateral cartilages are good candidates for autospreading.
The greatest challenge in performing primary aesthetic rhinoplasty is applying advanced evidence-based medicine with regard to anatomy, aesthetics, ethics, and ethnicity, to each individual case, and further customising the procedure to the individual face in order to provide the most natural result possible for the patient1, 2. Therefore, some principal criteria in the preoperative assessment of patients can be made to artistically improve the results. This must take into account the patient’s anatomy, deformities, nasofacial aesthetics, ethnicity, gender, and personal desires.
The endonasal (closed) and external (open) techniques are the two main techniques in primary and secondary rhinoplasty interventions, and are the most challenging procedures in modern aesthetic plastic surgery3, 4. For both approaches, the treatment goals are to preserve or achieve normal airflow and air-conditioning functions with primary aesthetic importance: aesthetically pleasing, natural appearance, retain ethnicity. Studies have reported that nasal obstruction is a relatively common problem in patients presenting for aesthetic rhinoplasty, with the prevalence of deviated nose syndrome5. The functions of the nose — specifically respiration, filtration, temperature regulation, and protection — are regulated by the septum, turbinates, and nasal valves (internal and external)5, 6.
Therefore, every rhinoplasty surgeon should cultivate a full understanding of intranasal and external anatomy7, the differential diagnosis of nasal obstruction, and the elements of a complete nasal examination (including nasal endoscopy); be comprehensive in the analysis of the facial and nasal regions; and have a broad understanding of the long-term effects of healing forces on the final nasal aesthetics and function5. Knowledge of medical and surgical rhinoplasty treatment options and anatomical side-effects can assist in anticipating certain surgical manoeuvres intraoperatively. In maximising nasal surgery safety issues, it is vital to have surgical procedure protocols, tools and equipment training for staff. Endotracheal anaesthesia care is preferable and a nasopharyngeal pack can be a useful preventive measure, helping to keep the larynx clear.
The aesthetic anatomy of the nose: dorsal aesthetic lines
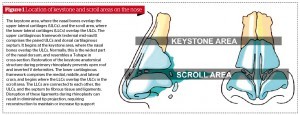
The bony cartilaginous pyramid of the external nose is a 3-dimentional structure composed of three basic regions: the upper rigid bony third, the middle semi-rigid cartilaginous third, and the lower mobile cartilaginous third. Common and uncommon nasal deformities usually result from a loss of tripod analogy support mechanisms4. The nasal–dorsal T-shape stabilisation keystone (K-area) is a critical area in which the quadrangular cartilage, nasal bones, perpendicular plate, and upper lateral cartilages (ULCs) come together8, forming the roof of the mid-nose (Figure 1).