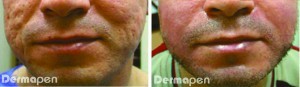
While active acne vulgaris itself can considerably reduce quality of life, the associated permanent disfiguring scars and their deleterious effect on appearance (and in some cases functionality) is usually behind the longer-lasting negative psychological impact on affected individuals. Fractional microneedle therapy with Dermapen® (Derma Pen LLC, Salt Lake City, Utah) provides a safe alternative to energy-based modalities for acne scarring, an indication for which it is FDA-cleared. It requires only topical anesthetic, and is virtually devoid of the risk of complications associated with effective energy-based alternatives such as fractional laser resurfacing.
The Dermapen
Dermapen is approximately the size of a large felt-tip marker. For any application, its disposable, sterile, single-use tip featuring an array of 11 microneedles causes minimally-traumatic fractional wounding in a pattern that is easily controlled by the operator. Needle penetration depth can be adjusted down to 0.25 mm, with piston stroke frequency adjustable to 90 Hz, giving Dermapen the capability of creating around 1000 minute wounds per second. During treatment the device is simply moved across the skin. As piston action (rather than pressure from the operator) drives needle penetration, wound depth is consistent from treatment to treatment, patient to patient. Treatment requires only topical anesthetic and is not energy-based, so there is virtually no limit to the number of therapy sessions one can safely undergo over time. The cost of the device and treatments is also much less than that of energy-based devices.
Literature review
While the entire body of microneedling literature may still be somewhat immature, no small portion of the research on microneedle therapy — also referred to as percutaneous collagen induction (PCI) — deals with its utility for scar revision. Seminal research by Orentreich and Orentreich in 19951 involved use of a tri-beveled hypodermic needle for scar subcision, and Camirand and Doucet’s 1997 study2 reported on the successful use of tattoo needles for scar revision.
More recent scientific treatment of PCI for acne scars using a dermal roller device by Fabbrocini et al3 described how fractionated microneedle wounding of the stratum corneum stimulated up-regulation of the healing cascade with minimal and transient disruption of the dermal barrier. As growth factors and other positive actors flood the area in response, fibroblast production and subsequent proliferation of keratinocytes instigates months of neocollagenesis, which builds skin volume in the treatment area. This is especially effective for low-grade macular scarring, rolling scars, and superficial boxcar scars.
Additional research by Fabbrocini et al, investigating acne scar treatment via dermal roller, has also been revealing. A 20094 study of 32 patients (20 women, aged 17–45 years) showed significant improvement in scar severity and overall aesthetic improvement after two microneedling sessions. Scar depth was evaluated by analysis of digital photography and, in a few cases, examining microrelief impressions made from silicone rubber. The treatment protocol included topical vitamin therapy for 3 weeks prior to the first session and no pigmentary complications were noted. In a 2010 trial5, subjects (n=60, 36 women, mean age 27 years, skin types I–VI) received three treatments at intervals of 4 to 12 weeks. In addition to demonstrating significant improvement in appearance, no incidence of pigmentary side-effects was noted — even in subjects of the darkest skin types.
Research into Dermapen versus dermal roller for atrophic acne scarring was presented at a 2012 medical conference6, bridging the gap between the technologies. All subjects (n=48) presented with predominantly rolling acne scars and had undergone previous treatment with dermal roller. Patients were randomied into two groups, one undergoing further dermal roller treatment, and the other undergoing treatment with Dermapen with assessment at 3 months. Both groups were assessed at 3 months. Visual assessment of improvement, as well as software analysis of digital scans, showed significantly greater scar improvement with Dermapen treatment. Patients reported via questionnaire that the treatment experience was much more tolerable and overall outcomes were better. Reported downtime, which for either therapy is relatively minimal and tolerable, was 1 or 2 days shorter, on average, with Dermapen. Operators reported that Dermapen was easier to use.
Safety is key
Although to date no research has directly compared fractional laser with Dermapen or similar fractional microneedle therapy, service as an alternative to the former may be the most compelling reason suggesting the use of Dermapen for acne scar revision. Fractional laser technology has certainly improved since it emerged on the market, and the modality is well-understood at this point, but specific issues have arisen during that time7. Among them, and perhaps most notoriously in recent times, is the potential incidence of post-inflammatory hyperpigmentation (PIH), especially in patients with skin of color2, owing to the character of the inflammatory cascade that results from induced thermal necrosis. Additionally, use of laser technology on darker skin has always required extreme care because of the prevalence of melanin as a competing chromophore.
Therapeutic damage inflicted by microneedling, especially in the case of Dermapen where the vertical insertion of needles causes the least possible trauma, causes apoptosis (programmed cell death), which has been shown to be well ordered histologically, with little or no excess inflammation because cell membranes remain intact for a time. Necrosis from thermal coagulation or ablation of tissue is more chaotic and replete with high levels of inflammation. By avoiding excess inflammation, microneedle therapy avoids the heightened risk of PIH seen with laser therapies8.
Additionally, because the therapeutic insult is minimally-traumatic and the epidermis is left largely intact during microneedle therapy, it can be repeated with little concern, as well as performed on patients and anatomical locations for which fractional laser therapy may be unsuitable9.